Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Childhood and Adolescent Mental Health section. Please contact Karen D. Wagner, MD, PhD, at [email protected].
Objectives: The aims of this study were to examine the symptoms of posttraumatic stress and anxiety/depression in Korean children after direct or indirect exposure to a single incident of trauma during a fire-escape drill and to assess the incidence of psychiatric disorders in this population.
Method: A total of 1,394 students who attended the elementary school at which the traumatic event took place were evaluated using self-administered questionnaires (the Child Posttraumatic Stress Disorder-Reaction Index [CPTSD-RI], State Anxiety Scale of the State-Trait Anxiety Inventory for Children [STAIC], and Children’s Depression Inventory [CDI]), as well as structured diagnostic interviews (Diagnostic Interview Schedule for Children, Version-IV [DISC-IV]) at 2 days (time point 1), 2 months (time point 2), and 6 months (time point 3) after the incident. The 335 students who witnessed the accident were defined as the direct-exposure group, and the remaining
students (n = 1,059) were defined as the indirect- exposure group. The study was conducted from May to November 2007.
Results: At time point 1, the prevalence of severe posttraumatic stress disorder (PTSD), anxiety, and depressive symptoms was 18.2%, 5.5%, and 3.4%, respectively. The prevalence of severe PTSD symptoms, as measured by the CPTSD-RI, was significantly higher in the direct-exposure group than in the indirect-exposure group (36.6% vs 12.7%, respectively; P < .001). At time point 2, the prevalence of severe PTSD symptoms was 7.4% (14.0% in the direct- exposure group and 4.9% in the indirect-exposure group, P < .001). The mean total CPTSD-RI score was significantly higher (P < .001) in the direct-exposure group than in the indirect-exposure group. At time point 3, thirty-eight of the 58 subjects (65.5%) evaluated with the DISC-IV in the direct-exposure group had 1 or more of the 7 anxiety/depressive disorders assessed, including subthreshold diagnoses. Among the diagnoses meeting full DSM-IV criteria for each disorder, agoraphobia was the most prevalent (22.4%), followed by generalized anxiety disorder (13.8%), separation anxiety disorder (6.9%), PTSD (5.2%), and social phobia (5.2%). When the subthreshold diagnoses were considered along with the full syndrome diagnoses, separation anxiety disorder was the most common diagnosis (41.4%), followed by agoraphobia (34.5%), obsessive-compulsive disorder (22.4%), PTSD (20.7%), and social phobia (20.7%).
Conclusions: The results of this study provide important evidence that various anxiety/depressive disorders, in addition to PTSD, might follow after direct or indirect exposure to trauma. Our findings highlight the importance of comprehensive screening for psychiatric problems in children exposed to trauma of any scale.
Submitted: November 25, 2008; accepted February 11, 2009.
Online ahead of print: June 16, 2009.
Corresponding author: Dr Jae-Won Kim, Department of Child and Adolescent Psychiatry, College of Medicine, Seoul National University Hospital, 28 Yongon-Dong, Chongno-Gu, Seoul, Korea ([email protected]).

A 6-Month Follow-Up Study of Posttraumatic Stress and Anxiety/Depressive Symptoms in Korean Children After Direct or Indirect Exposure to a Single Incident of Trauma
Objectives: The aims of this study were to examine the symptoms of posttraumatic stress and anxiety/depression in Korean children after direct or indirect exposure to a single incident of trauma during a fire-escape drill and to assess the incidence of psychiatric disorders in this population.
Method: A total of 1,394 students who attended the elementary school at which the traumatic event took place were evaluated using self-administered questionnaires (the Child Posttraumatic Stress Disorder-Reaction Index [CPTSD-RI], State Anxiety Scale of the State-Trait Anxiety Inventory for Children [STAIC], and Children’s Depression Inventory [CDI]), as well as structured diagnostic interviews (Diagnostic Interview Schedule for Children, Version-IV [DISC-IV]) at 2 days (time point 1), 2 months (time point 2), and 6 months (time point 3) after the incident. The 335 students who witnessed the accident were defined as the direct-exposure group, and the remaining students (n = 1,059) were defined as the indirect- exposure group. The study was conducted from May to November 2007.
Results: At time point 1, the prevalence of severe posttraumatic stress disorder (PTSD), anxiety, and depressive symptoms was 18.2%, 5.5%, and 3.4%, respectively. The prevalence of severe PTSD symptoms, as measured by the CPTSD-RI, was significantly higher in the direct-exposure group than in the indirect-exposure group (36.6% vs 12.7%, respectively; P < .001). At time point 2, the prevalence of severe PTSD symptoms was 7.4% (14.0% in the direct- exposure group and 4.9% in the indirect-exposure group, P < .001). The mean total CPTSD-RI score was significantly higher (P < .001) in the direct-exposure group than in the indirect-exposure group. At time point 3, thirty-eight of the 58 subjects (65.5%) evaluated with the DISC-IV in the direct-exposure group had 1 or more of the 7 anxiety/depressive disorders assessed, including subthreshold diagnoses. Among the diagnoses meeting full DSM-IV criteria for each disorder, agoraphobia was the most prevalent (22.4%), followed by generalized anxiety disorder (13.8%), separation anxiety disorder (6.9%), PTSD (5.2%), and social phobia (5.2%). When the subthreshold diagnoses were considered along with the full syndrome diagnoses, separation anxiety disorder was the most common diagnosis (41.4%), followed by agoraphobia (34.5%), obsessive-compulsive disorder (22.4%), PTSD (20.7%), and social phobia (20.7%).
Conclusions: The results of this study provide important evidence that various anxiety/depressive disorders, in addition to PTSD, might follow after direct or indirect exposure to trauma. Our findings highlight the importance of comprehensive screening for psychiatric problems in children exposed to trauma of any scale.
J Clin Psychiatry 2009;70(8):1148-1154
© Copyright 2009 Physicians Postgraduate Press, Inc.
Submitted: November 25, 2008; accepted February 11, 2009.
Online ahead of print: June 16, 2009 (doi:10.4088/JCP.08m04896).
Corresponding author: Dr Jae-Won Kim, Department of Child and Adolescent Psychiatry, College of Medicine, Seoul National University Hospital, 28 Yongon-Dong, Chongno-Gu, Seoul, Korea ([email protected]).
On May 17, 2007, two mothers of school children fell to their deaths from a height of more than 20 m when a basket attached to a fire engine ladder they were riding on swung abruptly after a wire connecting the ladder and the basket snapped. The women had been participating in a fire escape drill that was part of a family safety exercise program conducted at local elementary schools in Seoul, Republic of Korea, by the Seoul Metropolitan Fire and Disaster Management Department. Since its launch in 2006, the program has been conducted by fire departments from the city in 28 elementary schools. The program, which seeks to increase fire safety awareness, includes demonstrations of fire extinguishing, rescue operations, and first-aid administration. The 2 women had been participating in a rescue demonstration.
At the time of the accident, about 240 fourth grade students and their mothers, all of whom witnessed this event, were participating in this 3-hour program. Approximately 100 students who were looking out of their classroom windows also observed the accident.
It has been proposed that exposure to various types of traumatic events is associated with an increase in posttraumatic stress symptoms in children.1-3 Previous research has also reported an elevated prevalence of probable anxiety/depressive disorders after exposure to trauma.4 Researchers have explored the nature of trauma and the degree of exposure, as well as its relationship to posttraumatic stress reactions. Indirect trauma in children has also received clinical attention, since it has been suggested that it is associated with various psychiatric symptoms after the event.5
Several recent studies have proposed that indirect exposure is sufficient to induce posttraumatic stress disorder (PTSD) in vulnerable populations such as children and adolescents. Vila et al5 reported that the prevalence of PTSD in children indirectly exposed to a hostage-taking incident (children who were in the same school at the time of the incident but were not directly exposed to it) was 15%. In a study investigating the prevalence of posttraumatic stress symptoms in children attending school in London 6 months after the September 11, 2001, World Trade Center attack, 9% of the subjects were classified as having moderate to severe PTSD symptoms with functional impairment.6
With regard to childhood PTSD, Terr7 has proposed that Type I traumas (the result of a single and sudden traumatic event) differ from Type II traumas (the result of chronic and repeated traumas) in children and that the symptoms following Type I traumas are the typical features of PTSD in children. The majority of studies concerning Type I traumas in children have focused on their responses to direct exposure to natural disasters, transportation disasters, or terrorist attacks,1,3,8,9; few longitudinal data have been published with regard to how children respond to indirect traumas.
It should also be noted that previous studies of children and adolescents exposed to traumatic events have mainly focused on PTSD and have not assessed a range of psychiatric disorders. Moreover, few studies have used structured diagnostic instruments to evaluate mental disorders following traumatic events. Comparative studies of the differences in the impact or consequences of various levels of exposure to indirect traumas (eg, witnessing the event, hearing about the event) have not been conducted.
The aims of this study were to examine the symptoms of posttraumatic stress, anxiety, and depression following direct or indirect exposure to a single-incident of trauma in Korean children and to assess the incidence of psychiatric disorders in this population using structured diagnostic interviews. In addition, we tried to examine the impact of the trauma not only on the children who had witnessed the incident but also on the children who had been present at the school on the day of the accident but did not actually witness the event in order to compare the psychiatric consequences of direct and indirect exposure.
METHOD
Subjects and Procedure
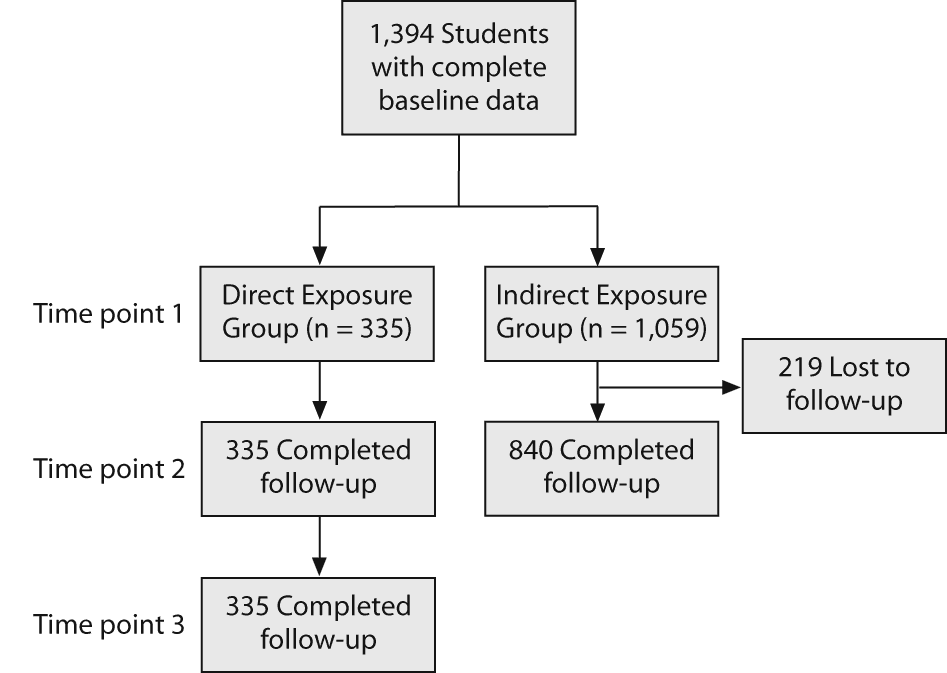
Figure 1 shows a flowchart of the study procedure. All of the children who attended the elementary school at which the accident took place (n = 1,456; first—sixth grade) were potential participants in this study. A total of 1,394 students who agreed to participate in this study and provided sufficient data were included in the statistical analysis (response rate = 95.7%). The first assessment was conducted 2 days after the incident (time point 1). Self-administered questionnaires—the Child Posttraumatic Stress Disorder-Reaction Index (CPTSD-RI),10 the State Anxiety Scale of the State-Trait Anxiety Inventory for Children (STAIC),11,12 and the Children’s Depression Inventory (CDI)13,14—were completed by each subject in the presence of experienced child and adolescent psychiatrists and master’s level psychologists (experienced in working with children and adolescents), who ensured that the subject understood the items. Subjects with severe posttraumatic stress symptoms (CPTSD-RI total score ≥ 40) or anxiety/depressive symptoms (State Anxiety Scale of the STAIC total score ≥ 49 or CDI total score ≥ 29) were identified as potential candidates for participation in the diagnostic interview using the Diagnostic Interview Schedule for Children, Version IV (DISC-IV).15,16 At time point 1, only the DISC-IV PTSD module was administered.
Figure 1. Participant Flow and Follow-Upa
aTime point 1 = 2 days after incident; time point 2 = 2 months after incident; time point 3 = 6 months after incident.
Click figure to enlarge
At time point 2 (2 months after the incident), the CPTSD-RI was administered to the subjects. A total of 1,175 students were evaluated (response rate = 84.3%) in this second assessment. There were no significant differences in demographic characteristics between the excluded and included subjects.
At time point 3 (6 months after the incident), self- report questionnaires (CPTSD-RI, State Anxiety Scale of the STAIC, and CDI) were first administered to the students who had witnessed the accident (direct-exposure group). A total of 335 students, 235 fourth grade students who had been participating in the fire escape drill and 100 students who had been looking out their classroom windows, were included. Subjects with severe symptoms of posttraumatic stress or anxiety/depression (applying the same cutoff points used at time point 1) were evaluated using the DISC-IV. Seven psychiatric disorders were assessed: PTSD, major depressive disorder, social phobia, separation anxiety disorder, agoraphobia, generalized anxiety disorder, and obsessive-compulsive disorder. The decision of which disorders should be included was based, in part, on the available posttrauma literature1,4 and the expert opinions of experienced child and adolescent psychiatrists.
The present study was approved by the Institutional Review Board for human subjects at Seoul National University Hospital in Korea. The parents of the subjects provided their written informed consent for the assessment of the children. The children or adolescents provided verbal assent to participate in the study.
Assessments
Child Posttraumatic Stress Disorder-Reaction Index. Posttraumatic stress disorder symptoms were evaluated using the 20-item self-report CPTSD-RI.10 Symptom frequency ratings were made on a 5-point Likert scale. The total CPTSD-RI score can range from 0 to 80, and a total score of 40 is considered the cutoff point for severe posttraumatic stress symptoms.
State Anxiety Scale of the State-Trait Anxiety Inventory for Children. The State Anxiety Scale of the STAIC consists of 20 self-rating questions that measure the level of anxiety.11 The State Anxiety Scale requires the subjects to describe how they feel at the present time and how their anxiety increases in response to situational stress and declines under relaxed conditions. The Korean version of the STAIC was standardized by Cho and Choi,12 who established a total score of 49 as the cutoff value for severe anxiety symptoms.
Children’s Depression Inventory. The CDI consists of 27 self-rating questions with a Likert scale of 0 (not present) to 2 (present and marked), and the total scores can range from 0 to 54.13 The item domains include negative mood, interpersonal problems, negative self-esteem, ineffectiveness, and anhedonia. The Korean version of the CDI was standardized in 1990, and its validity and reliability in Korean have been well established and previously reported.14 A total score of 29 is considered the cutoff point for severe depressive symptoms in the Korean version.
Diagnostic Interview Schedule for Children, Version IV. Psychiatric disorders diagnosed according to the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV)15 criteria were assessed using the Korean version of the DISC-IV. In this study, the DISC-IV scoring algorithms were derived from data provided by parents in order to ascertain the presence of a diagnosis. The test-retest reliability of the DISC-IV has been reported to be good.16 The reliability and validity of the Korean version of the DISC-IV were previously determined.17 For the diagnostic assessment of PTSD, we assessed both "full" PTSD (all DSM-IV criteria met) and "subthreshold" PTSD. At time point 1, the symptom duration was less than 1 month, and we therefore used the term "early" PTSD (PTSD without the duration criterion).18 Subthreshold PTSD was defined as having more than half of the required symptoms in each of the 3 symptom clusters (reexperiencing, avoidance, hyperarousal) or meeting full criteria for 2 of 3 symptom clusters.19 To meet subthreshold criteria using the DISC-IV PTSD module, symptoms also needed to be present for 1 month or longer following the event and to cause functional impairment. Subthreshold diagnoses were also provided for the other psychiatric disorders assessed. In brief, subthreshold diagnoses were made by including subthreshold symptoms that caused functional impairment, but not to the extent of the DSM-IV threshold level.
Statistical Analysis
Group differences in clinical variables involving continuous data were computed using an independent 2-sample t test or 1-way analysis of variance (ANOVA). Between-group comparisons involving categorical data were assessed using the χ2 test or Fisher exact test. The significance level was set at P = .05 (2-tailed). Changes in posttraumatic stress symptoms and anxiety/depressive symptoms were assessed using repeated measures ANOVA.
RESULTS
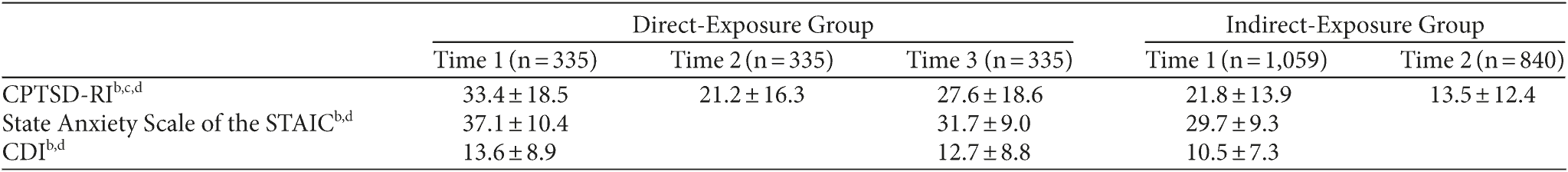
At time point 1, the prevalence of severe levels of PTSD, anxiety, and depressive symptoms was 18.2%, 5.5%, and 3.4%, respectively. The prevalence of severe PTSD symptoms, as measured by the CPTSD-RI, was significantly higher in the direct-exposure group than in the indirect-exposure group (36.6% vs 12.7%, respectively; P < .001). A total of 285 subjects (20.4%) participated in the diagnostic interview: 261 subjects (77.9%) from the direct-exposure group (n = 335) and 24 subjects (2.3%) from the indirect-exposure group (n = 1059). The prevalence of early PTSD diagnosed by the DISC-IV PTSD module was 10.9% (n = 31). An additional 39.6% of the children (n = 113) met the criteria for subthreshold early PTSD. The incidence of subthreshold early PTSD was significantly higher in the direct-exposure group than in the indirect-exposure group (χ2 = 3.88, P = .049). The boy:girl sex ratio for full syndrome early PTSD subjects was 1:1.7, and the ratio for subthreshold early PTSD was 1:0.9. With regard to the self-administered questionnaires, the mean total scores on the CPTSD-RI, State Anxiety Scale of the STAIC, and CDI were significantly higher (P < .001) in the direct-exposure group than in the indirect-exposure group (Table 1).
Table 1. Changes in CPTSD-RI, State Anxiety Scale of the STAIC, and CDI Scores According to Group and Timea
aAll values are expressed as mean ± SD.
bSignificant differences in between-group comparisons of CPTSD-RI, State Anxiety
Scale of the STAIC, and CDI scores at time points 1 and 2 (P < .001).
cSignificant differences in within-group comparisons of CPTSD-RI scores between time points 1 and 2 (P < .001).
dSignificant differences in within-group comparisons of CPTSD-RI, State Anxiety Scale of the STAIC, and CDI scores between time points 1 and 3 (P < .001, P < .001 and P = .021, respectively).
Abbreviations: CDI = Children’s Depression Inventory, CPTSD-RI = Child Posttraumatic Stress Disorder-Reaction Index; STAIC = State-Trait Anxiety Inventory for Children.
Click figure to enlarge
In the follow-up assessment at time point 2, the prevalence of severe PTSD symptoms was 7.4% (14.0% in the direct-exposure group and 4.9% in the indirect-exposure group, P < .001). The mean total CPTSD-RI score was significantly higher (P < .001) in the direct-exposure group than in the indirect-exposure group (Table 1).
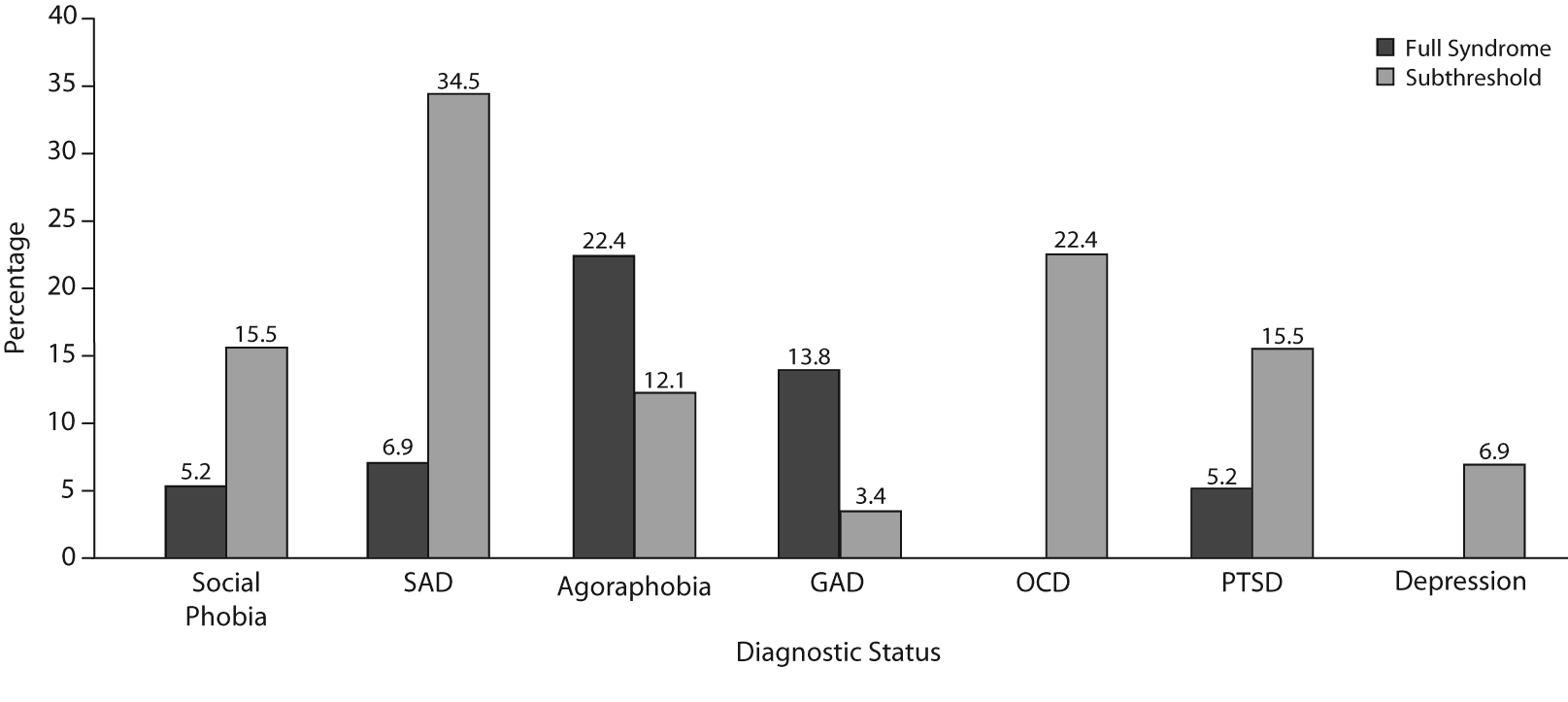
Figure 2. Rates of Full Syndrome and Subthreshold Diagnoses as Assessed by Structured Interviews in Children (n = 58) in the Direct-Exposure Group at 6-Month Follow-Up
Abbreviations: GAD = generalized anxiety disorder, OCD = obsessive-compulsive disorder, PTSD = posttraumatic stress disorder, SAD = separation anxiety disorder.
Click figure to enlarge
As shown in Figure 2 at time point 3, thirty-eight of the 58 subjects (65.5%) evaluated with DISC-IV had 1 or more of the 7 psychiatric disorders assessed, including subthreshold diagnoses. Among the diagnoses meeting full DSM-IV criteria for each disorder, agoraphobia was the most prevalent (22.4%), followed by generalized anxiety disorder (13.8%), separation anxiety disorder (6.9%), PTSD (5.2%), and social phobia (5.2%). When the subthreshold diagnoses were considered along with the full syndrome diagnoses, separation anxiety disorder was the most common (41.4%), followed by agoraphobia (34.5%), obsessive-compulsive disorder (22.4%), PTSD (20.7%), and social phobia (20.7%). The boy:girl sex ratio for the subjects who had 1 or more of the psychiatric diagnoses assessed was 1:2.5. The girls tended to have a higher prevalence of PTSD than the boys when the full syndrome and subthreshold diagnoses were considered together (χ2 = 2.91, P = .082).
Significant changes over time were detected in the results of self-administered questionnaires (Table 1). Between time points 1 and 2, within-group comparisons of scores showed a significant decrease in the mean total CPTSD-RI scores in both the direct and indirect-exposure groups (P < .001), and there was also a significant group difference (P = .001). Between time points 1 and 3, within-group comparisons of CPTSD-RI, State Anxiety Scale of the STAIC, and CDI scores were conducted in the direct-exposure group. The mean CPTSD-RI, State Anxiety Scale of the STAIC, and CDI scores significantly decreased over time (P < .001, P < .001 and P = .021, respectively).
DISCUSSION
In this study, at the baseline assessment (time point 1), 18.2% of the exposed children showed severe PTSD symptoms measured by the CPTSD-RI, regardless of whether they actually witnessed the event. Approximately half (51.5%) of the subjects who participated in the diagnostic interview at time point 1 were diagnosed as having early PTSD, when full early PTSD (10.9%) and subthreshold early PTSD (39.6%) were considered together. Severe levels of anxiety or depressive symptoms were also reported in the exposed children. At time point 2, only the CPTSD-RI was administered to the subjects, and the results showed a decrease in the prevalence of severe PTSD symptoms to 7.4%.
In our study, at time point 1, we used the definition of "early" PTSD (PTSD without the duration criterion)18 instead of acute stress disorder or subacute stress disorder (acute stress disorder minus the dissociation criterion),20 since we used the DISC-IV PTSD module for the diagnostic assessment. Although PTSD and acute stress disorder share similar symptom clusters and impairment criteria, the specific symptom numbers or intensities required for diagnosis vary, and, most of all, additional dissociative symptoms are specified in acute stress disorder. Unfortunately, posttraumatic dissociative reactions were not examined in this study.
Our results are comparable to those reported in recent posttrauma studies. Eight weeks after a tsunami struck Thailand, the prevalence of PTSD symptoms in children living in displacement camps, affected villages, and unaffected villages was 13%, 11%, and 6%, respectively.3 Following a 1999 earthquake in Greece, the estimated incidence of PTSD was 5% after 3 months.21 However, the instruments used to measure PTSD symptoms in the previously mentioned studies were different from the one used in our study, and, therefore, it may be inappropriate to compare the results without adjusting for any demographic or clinical differences that might exist among the samples of each study. It is worth noting that our assessment of PTSD symptoms at time point 2 was critical, since it has been suggested that acute manifestations of psychiatric problems have either disappeared or become more permanent by 8 weeks posttrauma.
Our findings extend the growing body of evidence suggesting that individuals may experience PTSD symptoms after viewing distressing scenes or media footage, such as those of the traumatic events that took place on September 11, 2001.6,19 In other words, regarding the responses of children to exposure to indirect traumas, there is a possibility that subjects might have a clinical level of posttraumatic stress symptoms, regardless of whether they are directly exposed (eg, witnessed the event involving death or serious injury) or indirectly exposed (eg, did not witness death or injury but were exposed to media-based coverage or heard about it) to the traumatic event.
Recent studies have shown that children can suffer from PTSD symptoms without meeting the traumatic event criterion of the DSM-IV,5,22 which was the case for the indirect-exposure group in this study. Although the subjects’ scores on the self-administered questionnaires were lower in the indirect-exposure group than in the direct-exposure group at time points 1 and 2, it is worth noting that 12.7% of the subjects from the indirect-exposure group at time point 1 and 4.9% at time point 2 had severe PTSD symptoms. The results of this study suggest that population-based screening for mental health problems in children after traumatic events should include those who are indirectly exposed to the trauma. As proposed by Schwarz,23 the level of subjective involvement and the intensity of emotional reactions may play a role in determining the "exposure" to any specific kind of trauma, and these criteria are as important as the physical proximity to the vital threat.
One of our main findings was that a wide range of anxiety/depressive disorders were identified in addition to PTSD at the follow-up assessment in the subjects who had directly witnessed the accident. At the 6-month follow-up, 38 subjects (11.3%) in the direct-exposure group (n = 335) had 1 or more of the 7 psychiatric disorders assessed, either full syndrome or subthreshold diagnoses, as evaluated by the DISC-IV. In a recent study by Vila et al.,5 the Kiddie Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS) was used for the diagnosis of DSM-IV psychiatric disorders. During the follow-up period, in addition to PTSD, separation anxiety disorder (n = 3) and major depressive disorder (n = 2) were diagnosed in a sample of directly exposed children. However, the sample size of that study was smaller than that of our study. In a prevalence study of psychopathology among school children 6 months after the September 11, 2001, World Trade Center attack, 28.6% of all children had 1 or more of the 6 probable anxiety/depressive disorders.4 The most prevalent disorders in that sample were probable agoraphobia, followed by probable separation anxiety disorder and probable PTSD. The results of that study are comparable to those of ours, which also identified agoraphobia and separation anxiety disorder as the main psychiatric diagnoses. However, supposedly because of the nature of their population-based survey with a large sample size, the Diagnostic Interview Schedule for Children Predictive Scales, instead of structural diagnostic interviews, was used to assess probable psychiatric disorders.
In a 9-month follow-up study examining the effects of motor vehicle accidents, Keppel-Benson et al24 reported rates of PTSD and specific phobia of 14% and 10%, respectively, from a structured diagnostic interview using the Diagnostic Interview for Children and Adolescents. A longitudinal epidemiologic study, which used the Child and Adolescent Psychiatric Assessment to evaluate psychiatric disorders in children, reported that trauma exposure, apart from PTSD, was related to the lifetime occurrence of a variety of psychopathologies, with the strongest links being to depression and anxiety disorders.25 In addition to the previously mentioned anxiety/depressive disorders following traumatic events, researchers also focused on other behavioral/emotional problems as long-term consequences of childhood trauma, including attachment problems, disruptive behavior disorders, alcohol and substance abuse, and eating disorders.26,27
The variety of psychiatric disorders observed in the follow-up assessment of this study highlights the importance of comprehensive screening for psychiatric problems in children exposed to trauma of any scale. Our data may be useful for targeting mental health services toward children and adolescents after various traumatic events, including indirect traumas.
Several limitations to this study should be noted. First, it may be inappropriate to generalize the results of this study to children affected by other kinds of traumatic events.
Second, we did not examine the various psychosocial factors that might influence how children respond to trauma. The family factor is one such factor, and it has been proposed that individual factors may interact with factors in the family, leading to the development of posttraumatic stress symptoms or other psychiatric symptoms.28 Parental psychopathology, mother-child relationship, or family stress, which are examples of several notable factors reported in PTSD literature, were not evaluated in this study. Parental trauma exposure or parental PTSD were not assessed, which has the limitation of precluding an evaluation of the relationships between these parental conditions and the occurrence of psychiatric symptoms in their children. Recent studies suggested parental trauma exposure and PTSD as putative risk factors for the development of PTSD, depression, and anxiety disorders in offspring.29
Third, regarding individual factors, the preincident psychiatric status of the children, including preexisting psychiatric disorders, was not examined in our sample. Fourth, we did not examine the nature or degree of exposure, as well as its relationship with the posttraumatic reactions in children and their families.
Finally, structured diagnostic interviews were administered only to the direct-exposure group at the 6-month follow-up, and we were unable to assess the incidence or prevalence of psychiatric disorders in the indirect-exposure group. At the 6-month follow-up, the school principal and most of the parents from the indirect-exposure group were extremely concerned about administrating the self-report measures, including the measure of PTSD, and the possible distressing effects on children, such as reexperiencing the incident; these concerns prevented a follow-up assessment’s being carried out at time point 3 for the indirect-exposure group. Further studies are needed in order to identify the relationship between the level of exposure to indirect trauma and the likelihood of various anxiety/depressive disorders in children.
CONCLUSIONS
The results of this study provide important evidence that various anxiety/depressive disorders, in addition to PTSD, might follow after direct or indirect exposure to indirect trauma. Our findings highlight the importance of comprehensive screening for psychiatric problems in children exposed to trauma of any scale.
Author affiliations: The Department of Child and Adolescent Psychiatry, College of Medicine, Seoul National University Hospital, Seoul, Republic of Korea (Drs B.-N. Kim, J.-W. Kim, H.-W. Kim, Shin, and Cho); Seoul Women’s College of Nursing & Seoul Institute for Narrative Studies (Dr Choi); Department of Psychology, College of Social Sciences, Ewha Womans University (Drs Ahn and Lee); Cognitive Science Program, Graduate School, Yonsei University & Seoul Institute for Narrative Studies (Ms Ryu); and the Seoul Metropolitan Child and Adolescent Mental Health Center (Ms Yun).
Financial disclosure: Drs B.-N. Kim, J.-W. Kim, H.-W. Kim, Shin, Cho, Choi, Ahn, and Lee and Mss Ryu and Yun report no financial or other relationships relevant to the subject of this article.
Funding/support: None reported.
REFERENCES
1. Goenjian AK, Molina L, Steinberg AM, et al. Posttraumatic stress and depressive reactions among Nicaraguan adolescents after hurricane Mitch. Am J Psychiatry. 2001;158(5):788-794. PubMed doi:10.1176/appi.ajp.158.5.788
2. McDermott BM, Doughty DE, Reddy C, et al. Posttraumatic stress disorder and general psychopathology in children and adolescents following a wildfire disaster. Can J Psychiatry. 2005;50(3):137-143. PubMed
3. Thienkrua W, Cardozo BL, Chakkraband MLS, et al Thailand Post-Tsunami Mental Health Study Group. Symptoms of posttraumatic stress disorder and depression among children in tsunami-affected areas in southern Thailand. JAMA. 2006;296(5):549-559. PubMed doi:10.1001/jama.296.5.549
4. Hoven CW, Duarte CS, Lucas CP, et al. Psychopathology among New York city public school children 6 months after September 11. Arch Gen Psychiatry. 2005;62(5):545-552. PubMed doi:10.1001/archpsyc.62.5.545
5. Vila G, Porche LM, Mouren-Simeoni MC. An 18-month longitudinal study of posttraumatic disorders in children who were taken hostage in school. Psychosom Med. 1999;61(6):746-754. PubMed
6. Holmes EA, Creswell C, O’ Connor TG. Posttraumatic stress symptoms in London school children following September 11, 2001: an exploratory investigation of peri-traumatic reactions and intrusive imagery. J Behav Ther Exp Psychiatry. 2007;38(4):474-490. PubMed doi:10.1016/j.jbtep.2007.10.003
7. Terr LC. Childhood traumas: an outline and overview. Am J Psychiatry. 1991;148(1):10-20. PubMed
8. de Vries AP, Kassam-Adams N, Cnaan A. Looking beyond the physical injury: posttraumatic stress disorder in children and parents after pediatric traffic injury. Pediatrics. 1999;104(6):1293-1299. PubMed doi:10.1542/peds.104.6.1293
9. Koplewicz HS, Vogel JM, Solanto MV, et al. Child and parent response to the 1993 World Trade Center bombing. J Trauma Stress. 2002;15(1):77-85. PubMed doi:10.1023/A:1014339513128
10. Steinberg AM, Brymer MJ, Decker KB, et al. The University of California at Los Angeles Posttraumatic Stress Disorder Reaction Index. Curr Psychiatry Rep. 2004;6(2):96-100. PubMed doi:10.1007/s11920-004-0048-2
11. Spielberger CD. Manual for the State-Trait Anxiety Inventory for Children. Palo Alto, CA: Consulting Psychological Press; 1972.
12. Cho SC, Choi JS. Development of the Korean version of State-Trait Anxiety Inventory for Children. Seoul Rev Psychiatry. 1989;14:150-157.
13. Kovacs M. The Children’s Depression Inventory. Psychopharmacol Bull. 1985;21(4):995-998. PubMed
14. Cho SC, Lee YS. Development of the Korean version of Children’s Depression Inventory. J Korean Neuropsychiatr Assoc. 1990;29:943-956.
15. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: American Psychiatric Association; 1994.
16. Shaffer D, Fisher P, Lucas CP, et al. NIMH Diagnostic Interview Schedule for Children, Version IV (NIMH DISC-IV): description, differences from previous versions, and reliability of some common diagnoses. J Am Acad Child Adolesc Psychiatry. 2000;39(1):28-38. PubMed doi:10.1097/00004583-200001000-00014
17. Cho SC, Kim BN, Kim JW, et al. The reliability and validity of Diagnostic Interview Schedule for Children, Version IV – Korean Version (DISC-IV). J Kor Acad Child Adolesc Psychiatry. 2007;18:138-144.
18. Meiser-Stedman R, Yule W, Smith P, et al. Acute stress disorder and posttraumatic stress disorder in children and adolescents involved in assaults or motor vehicle accidents. Am J Psychiatry. 2005;162(7):1381-1383. PubMed doi:10.1176/appi.ajp.162.7.1381
19. Otto MW, Henin A, Hirshfeld-Becker DR, et al. Posttraumatic stress disorder symptoms following media exposure to tragic events: impact of 9/11 on children at risk for anxiety disorders. J Anxiety Disord. 2007;21(7):888-902. PubMed doi:10.1016/j.janxdis.2006.10.008
20. Harvey AG, Bryant RA. Acute stress disorder: a synthesis and critique. Psychol Bull. 2002;128(6):886-902. PubMed doi:10.1037/0033-2909.128.6.886
21. Roussos A, Goenjian AK, Steinberg AM, et al. Posttraumatic stress and depressive reactions among children and adolescents after the 1999 earthquake in Ano Liosia, Greece. Am J Psychiatry. 2005;162(3):530-537. PubMed doi:10.1176/appi.ajp.162.3.530
22. Nader K, Pynoos R, Fairbanks L, et al. Children’s PTSD reactions one year after a sniper attack at their school. Am J Psychiatry. 1990;147(11):1526-1530. PubMed
23. Schwarz ED. The post-traumatic response in children and adolescents. Psychiatr Clin North Am. 1994;17(2):311-326. PubMed
24. Keppel-Benson JM, Ollendick TH, Benson MJ. Post-traumatic stress in children following motor vehicle accidents. J Child Psychol Psychiatry. 2002;43(3):203-212. PubMed doi:10.1111/1469-7610.00013
25. Copeland WE, Keeler G, Angold A, et al. Traumatic events and posttraumatic stress in childhood. Arch Gen Psychiatry. 2007;64(5):577-584. PubMed doi:10.1001/archpsyc.64.5.577
26. Perry BD, Azad I. Posttraumatic stress disorders in children and adolescents. Curr Opin Pediatr. 1999;11(4):310-316. PubMed doi:10.1097/00008480-199908000-00008
27. Pine DS, Cohen JA. Trauma in children and adolescents: risk and treatment of psychiatric sequelae. Biol Psychiatry. 2002;51(7):519-531. PubMed doi:10.1016/S0006-3223(01)01352-X
28. Silva RR, Alpert M, Munoz DM, et al. Stress and vulnerability to posttraumatic stress disorder in children and adolescents. Am J Psychiatry. 2000;157(8):1229-1235. PubMed doi:10.1176/appi.ajp.157.8.1229
29. Yehuda R, Halligan SL, Bierer LM. Relationship of parental trauma exposure and PTSD to PTSD, depressive and anxiety disorders in offspring. J Psychiatr Res. 2001;35(5):261-270. PubMed doi:10.1016/S0022-3956(01)00032-2
Enjoy this premium PDF as part of your membership benefits!