Prim Care Companion CNS Disord 2021;23(6):21br03028
To cite: Uvais NA. COVID-19 vaccine hesitancy among patients with psychiatric disorders. Prim Care Companion CNS Disord. 2021;23(6):21br03028.
To share: https://doi.org/10.4088/PCC.21br03028
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Department of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India ([email protected]).
In the absence of any effective treatment for coronavirus disease 2019 (COVID-19) infection, the only option currently considered as the most important step in the control of the pandemic is the COVID-19 vaccination. However, the effectiveness of any vaccination program depends on the uptake of the vaccination by a significant section of the population.1 Studies2 have shown that 67% vaccination coverage is needed to achieve herd immunity against COVID-19 infection. Vaccine hesitancy is defined as a behavioral pattern of delay in acceptance or refusal of vaccine in spite of vaccine availability.3 Research from across the world has shown a varying pattern of COVID-19 vaccine hesitancy among the general population.4 Vaccine hesitancy has also been found to be influenced by confidence in vaccine and/or provider, complacency, and convenience to access the vaccination.5 There is a significant level of public uncertainty in many countries regarding various COVID-19 vaccine candidates due to multiple factors including the rapid development and novelty of the vaccine, poor communication from government and policymakers regarding the efficacy and safety of the vaccine, and poor clinical trial data transparency.5
People with psychiatric illnesses are at higher risk of COVID-19 infection and associated complications due to multiple factors.6 Comorbid medical conditions, altered immune functions, sleep-related problems, and various socioeconomic risk factors contribute to the higher rate of COVID-19 infection and worse outcomes in people with psychiatric disorders.6 Studies7,8 from around the world clearly found significant association between an existing psychiatric disorder and increased risk for COVID-19 infection and COVID-19–related hospitalization, morbidity, and mortality. The prognosis has been found to be worse among patients with severe mental illness (SMI) than for those with less severe SMI.7,8 Therefore, patients with psychiatric disorders should be considered a vulnerable group for COVID-19 infection and must be provided early access to COVID-19 vaccination.
Vaccine hesitancy among patients with psychiatric disorders is a less explored area. There are only a few studies among patients with psychiatric disorders evaluating the rate of vaccine uptake or willingness of patients to receive vaccinations. Previous studies9 done during the influenza pandemic showed very low vaccination uptake among patients with SMI. However, the majority of the patients with SMI believed in the safety and effectiveness of the vaccine and that vaccinations are safe and effective in general, and 74% reported moderate willingness to receive vaccination.10,11 Apart from vaccine hesitancy, factors such as lack of knowledge and awareness, accessibility problems, costs, fears about immunization, and poor recommendations from health care providers also contribute to the low vaccination rate among patients with psychiatric disorders.6 To the best of my knowledge, there are no studies evaluating COVID-19 vaccination hesitancy among patients with psychiatric disorders. This study is a preliminary attempt to understand COVID-19 vaccine hesitancy among Indian patients with various psychiatric disorders.
Methods
The objective of this hospital-based cross-sectional study was to examine COVID-19 vaccination hesitancy among patients with mental illness. The study was conducted from March 29, 2021, to April 21, 2021. All consecutive patients attending an outpatient psychiatry department in a tertiary care hospital in Kerala, India were enrolled in the study after obtaining informed consent. The questionnaire consisted of questions in English alongside its Malayalam translation. The questionnaire consisted of demographic details, COVID-19 experience and health self-assessment, and a structured questionnaire to assess the acceptability of COVID-19 vaccination and preferences. The intention to receive vaccination was assessed using a direct leading question with a 4-point scale (definitely no, probably no, probably yes, definitely yes), while preferences regarding local or imported vaccines were rated using another 4-point scale (completely confident to completely not confident).
Data were analyzed using Statistical Package for Social Sciences version 14 (SPSS Inc, Chicago, Illinois). Frequencies and percentages were used to describe the data. χ2 was applied to determine statistical differences between groups. The resulting P values were considered significant if < .05.
Results
Responses were received from 90 patients with psychiatric illness. The majority of the participants (80%) were aged 26–60 years, 58.9% were female, and 75.6% were married. Sixty percent of the participants studied up to high school (< 10 years of formal education), and only 34.4% were employed at the time of the study. Also, 77.8% of the participants were Muslim, 62.9% earned a family income < ₹25,000 (< US $335)/mo, 66.7% were living in a rural area, and 32.2% had other comorbid medical illnesses. Only 6.7% of the participants had been infected with COVID-19, but 16.7% had a history of COVID-19 infection among their close relatives or friends. Further, 75.6% of the study population rated their overall health as good or very good. The sociodemographic variables are summarized in Table 1.
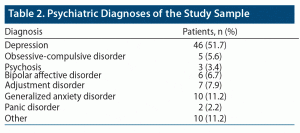
The most common diagnosis of the study sample was depressive disorder (51.7%), followed by generalized anxiety disorder (11.2%), adjustment disorder (7.9%), bipolar affective disorder (6.7%), and obsessive-compulsive disorder (5.6%). The diagnoses of the study participants are summarized in Table 2.
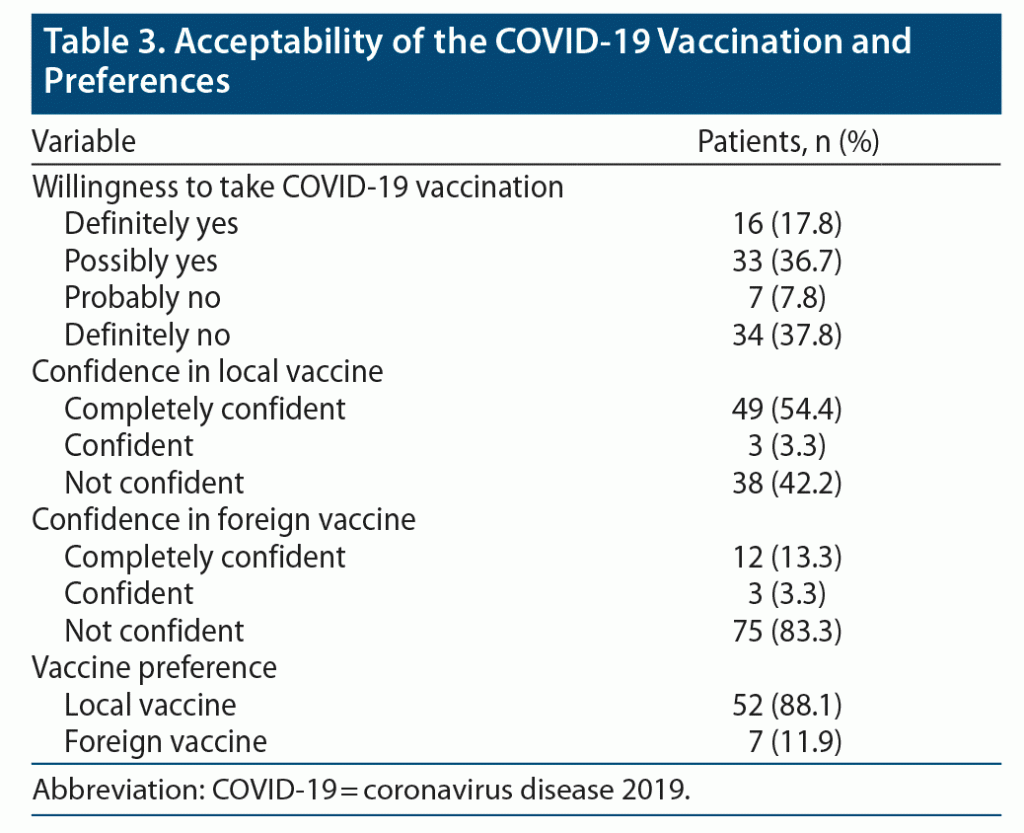
Regarding willingness to receive COVID-19 vaccination, only 17.8% reported a definitive intention to receive vaccination, and 37.8% reported a definitive intention not to receive vaccination. Also, 36.7% reported that they would probably receive vaccination, and 7.8% reported that they probably would avoid receiving vaccination. While 54.4% of the study sample reported that they have complete confidence in locally made COVID-19 vaccine, only 13.3% reported complete confidence in foreign-made vaccine; 88.1% preferred locally made COVID-19 vaccine over foreign-made COVID-19 vaccine. The acceptability of COVID-19 vaccination and preferences are summarized in Table 3. There was a statistically significant association between intention to receive COVID-19 vaccination and education level, with a higher rate of definitive intention to receive COVID-19 vaccination among participants with higher educational achievements (χ26 = 14.83, P = .015). There was a statistically significant association between religion and intention to receive COVID-19 vaccination (P < .05), with participants belonging to the religion of Islam reporting a significantly higher definitive intention to not take the COVID-19 vaccine. There was no statistically significant difference in vaccination intention between patients with neurotic spectrum disorder and psychotic spectrum disorder.
Discussion
Promotion of COVID-19 vaccine uptake among vulnerable populations such as patients with psychiatric illnesses is an important public health priority at the moment, as emerging evidence clearly indicates that patients with psychiatric conditions are prone to higher rates of COVID-19 infection as well as its complications. This study explored COVID-19 vaccination hesitancy among Indian patients with psychiatric disorders. Findings of this study showed that only 54.5% of the respondents reported a definitive or probable intention to receive COVID-19 vaccination, and 37.8% reported a definitive intention not to receive vaccination. The COVID-19 vaccination hesitancy in this study is significantly higher when compared to studies conducted among the general population across the world. A recent global survey exploring acceptance of COVID-19 vaccine among the population of 19 countries found an overall 71.5% acceptance for COVID-19 vaccination uptake.12 A systematic review of studies on COVID-19 vaccination acceptance conducted in 33 countries across the globe also found3 a 70% acceptance rate in the majority of the studies.13 In summary, there is a significantly higher vaccine hesitancy among patients with psychiatric illnesses compared to the general population. Public health experts and policymakers should reach out to this vulnerable population with specific public health interventions to target COVID-19 vaccine hesitancy among this group.
This study also showed a significantly higher confidence and preference for locally manufactured COVID-19 vaccines over foreign-made imported vaccines. Considering that India is a major vaccine manufacturer, confidence in Indian-made COVID-19 vaccination among the studied population has many public health benefits. It will be more economical and feasible for government agencies to provide locally made COVID-19 vaccines to the local population compared to imported COVID-19 vaccines. Public health outreach activities with transparent data regarding the effectiveness and safety of locally made vaccine candidates might significantly decrease COVID-19 vaccine hesitancy among Indian patients with psychiatric illnesses.
This study also found that the intention to receive COVID-19 vaccination is significantly higher among patients with higher educational attainment. Previous studies exploring COVID-19 vaccine hesitancy among the general population also found that intention of refusing to take of the COVID-19 vaccine was significantly higher in individuals with lower levels of education.14,15 Moreover, religious beliefs have also been found to significantly influence COVID-19 vaccination intention. Respondents belonging to the religion of Islam reported significantly higher vaccine hesitancy. Research exploring COVID-19 vaccination hesitancy found significantly lower COVID-19 vaccine acceptance in some Middle Eastern countries with majority Muslim populations.13 Another contributing factor for vaccine hesitancy among Muslims could be the misleading news claiming that traces of pork are used in the development of COVID-19 vaccines. Although scholars of Islamic ethics argued that vaccines produced using chemically transformed pork may be permissible, many fatwas circulated on social media platforms advising Muslims to avoid the Chinese vaccine against COVID-19, which was believed to be manufactured with an ingredient derived from pork.16
In conclusion, this study has important implications for promoting COVID-19 vaccination uptake among Indian patients with psychiatric conditions. It is recommended that tailored public health interventions targeting vaccine hesitancy among this vulnerable population should be prioritized to prevent higher rates of COVID-19 infection and mortality in this high-risk group.
Received: May 30, 2021.
Published online: November 4, 2021.
Potential conflicts of interest: None.
Funding/support: None
References (16)

- Lin Y, Hu Z, Zhao Q, et al. Understanding COVID-19 vaccine demand and hesitancy: a nationwide online survey in China. PLoS Negl Trop Dis. 2020;14(12):e0008961. PubMed CrossRef
- Randolph HE, Barreiro LB. Herd immunity: understanding COVID-19. Immunity. 2020;52(5):737–741. PubMed CrossRef
- Kumar D, Chandra R, Mathur M, et al. Vaccine hesitancy: understanding better to address better. Isr J Health Policy Res. 2016;5(1):2. PubMed CrossRef
- Alobaidi S. Predictors of intent to receive the COVID-19 vaccination among the population in the Kingdom of Saudi Arabia: a survey study. J Multidiscip Healthc. 2021;14:1119–1128. PubMed CrossRef
- Smith K, Lambe S, Freeman D, et al. COVID-19 vaccines, hesitancy and mental health. Evid Based Ment Health. 2021;24(2):47–48. PubMed CrossRef
- Mazereel V, Van Assche K, Detraux J, et al. COVID-19 vaccination for people with severe mental illness: why, what, and how? Lancet Psychiatry. 2021;8(5):444–450. PubMed CrossRef
- Nemani K, Li C, Olfson M, et al. Association of psychiatric disorders with mortality among patients with COVID-19. JAMA Psychiatry. 2021;78(4):380–386. PubMed CrossRef
- Lee SW, Yang JM, Moon SY, et al. Association between mental illness and COVID-19 susceptibility and clinical outcomes in South Korea: a nationwide cohort study. Lancet Psychiatry. 2020;7(12):1025–1031. PubMed CrossRef
- Lorenz RA, Norris MM, Norton LC, et al. Factors associated with influenza vaccination decisions among patients with mental illness. Int J Psychiatry Med. 2013;46(1):1–13. PubMed CrossRef
- Maguire PA, Reay RE, Looi JC. Nothing to sneeze at—uptake of protective measures against an influenza pandemic by people with schizophrenia: willingness and perceived barriers. Australas Psychiatry. 2019;27(2):171–178. PubMed CrossRef
- Miles LW, Williams N, Luthy KE, et al. Adult vaccination rates in the mentally ill population: an outpatient improvement project. J Am Psychiatr Nurses Assoc. 2020;26(2):172–180. PubMed CrossRef
- Lazarus JV, Ratzan SC, Palayew A, et al. A global survey of potential acceptance of a COVID-19 vaccine. Nat Med. 2021;27(2):225–228. PubMed CrossRef
- Sallam M. COVID-19 vaccine hesitancy worldwide: a concise systematic review of vaccine acceptance rates. Vaccines (Basel). 2021;9(2):160. PubMed CrossRef
- Kanozia R, Arya R. “Fake news”, religion, and COVID-19 vaccine hesitancy in India, Pakistan, and Bangladesh [published online ahead of print May 17, 2021]. Media Asia. 2021. CrossRef
- Soares P, Rocha JV, Moniz M, et al. Factors associated with COVID-19 vaccine hesitancy. Vaccines (Basel). 2021;9(3):300. PubMed CrossRef
- Ghaly M. Islamic Ethics, COVID-19 Vaccination, and the Concept of Harm. The Hastings Center. 2021. https://www.thehastingscenter.org/islamic-ethics-covid-19-vaccination-and-concepts-of-harm/
Enjoy this premium PDF as part of your membership benefits!