ABSTRACT
Objective: Prolongation of corrected QT (QTc) interval increases the risk of severe ventricular arrhythmias, in particular torsades de pointes. Patients with severe mental illness (SMI) represent a vulnerable population. This study aimed to measure the prevalence of QTc prolongation in inpatients with SMI and to identify risk factors for QTc prolongation.
Methods: Demographic, clinical, anthropometric, laboratory, and electrocardiographic information was extracted from the electronic records of a cohort of patients hospitalized in a psychiatry inpatient unit between July 1, 2017, and July 22, 2019. The primary outcome was the estimation of prevalence of QTc prolongation. The secondary outcome was the identification of risk factors for QTc prolongation.
Results: A total of 597 admissions were included. Only 1.4% had a QTc > 500 msec, while 11.6% had a QTc > 460 msec. The proportion of women with a QTc > 470 msec was 3.6% and men with a QTc > 450 msec was 7.3%. Several risk factors were individually associated with QTc prolongation. In the multivariate model explaining almost one-third of QTc variance, female sex (P = .04), older age (P = .011), heart rate (P < .001), systolic blood pressure (P = .042), potassium (P = .012), hemoglobin (P = .006), number of antipsychotics (P = .026), and treatment with clotiapine (P = .012) and clozapine (P = .003) were associated with QTc length. Several factors beyond pharmacologic treatment identify subjects at risk for QTc prolongation, and polypharmacotherapy does not seem to increase the risk of QTc prolongation.
Conclusions: QTc prolongation was rare in this cohort of SMI inpatients. Most of the risk factors involved in QTc prolongation are unchangeable elements or linked to general medical conditions, and only a few are modifiable factors, including psychotropic treatment.
Prim Care Companion CNS Disord 2022;24(1):21m02915
To cite: Salvati B, Miola A, Toffanin T, et al. Prevalence and risk factors for QTC prolongation in acute psychiatric hospitalization. Prim Care Companion CNS Disord. 2022;24(1):21m02915.
To share: https://doi.org/10.4088/PCC.21m02915
© Copyright 2022 Physicians Postgraduate Press, Inc.
aDepartment of Neuroscience, University of Padova, Padua, Italy
bPadua University Hospital, Padua, Italy
cPadova Neuroscience Center, University of Padova, Padua, Italy
dDepartment of Psychiatry, University of Ottawa, Ontario, Canada
eDepartment of Mental Health, The Ottawa Hospital, Ontario, Canada
fOttawa Hospital Research Institute (OHRI) Clinical Epidemiology Program, University of Ottawa, Ottawa, Ontario, Canada
gSchool of Epidemiology and Public Health, Faculty of Medicine, University of Ottawa, Ottawa, Canada
‡These authors contributed equally to this work.
*Corresponding author: Alessandro Miola, MD, Department of Neuroscience, University of Padova, Padua, Italy, Via Giustiniani, 5, Padua, Italy ([email protected]).
According to the literature, there is an association between antipsychotic drugs and prolongation of corrected QT (QTc) interval with Bazett’s formula.1–4 QTc interval represents an indirect marker of potential proarrhythmic toxicity, in particular of polymorphic ventricular arrhythmia called torsades de pointes (TdP), which can evolve into ventricular fibrillation and cause sudden cardiac death. While there is no international agreement on a safety threshold for the QTc interval, a consensus was reached considering QTc intervals > 440 msec as normal5 and QTc prolongation > 500 msec as at increased risk for TdP.2
Among other factors, psychotropic drugs have been shown to be associated with QTc prolongation. Both first-generation antipsychotics (FGAs) and second-generation antipsychotics (SGAs) are associated with QTc interval prolongation,6 with SGAs being safer than FGAs,7 with few exceptions.3,8 The relationship between drug dose and risk of QTc interval prolongation is controversial,7,9 and the relationship between antipsychotic polypharmacy and QTc remains uncertain.2,4,10 QTc interval can also be significantly influenced by the route of administration of antipsychotic drug, with parenteral being less safe than oral administration, particularly for haloperidol.11,12 Antidepressants have also raised concerns regarding the risk of QTc prolongation. More specifically, selective serotonin reuptake inhibitors (SSRIs) appear to be safe in general, with the exception of citalopram and escitalopram, which have a dose-dependent predictable negative effect on the QTc.13 Tricyclic antidepressants (TCAs) are significantly associated with serious cardiovascular side effects, including prolongation of the QTc interval.14 Among mood stabilizers, lithium in blood concentrations greater than 1.2 mmol/L may prolong the QTc interval, although no cases of TdP have been reported.15 No risk of QTc prolongation with valproate or lamotrigine has been reported to the best of our knowledge.
In addition to psychotropic drugs, numerous other factors have been recognized as affecting QT interval, including both congenital and acquired conditions, as well as the use of various other drugs (antibiotics, antiarrhythmics, antifungal agents, methadone).3 The primary aim of this study was to measure the prevalence of QTc interval prolongation in a real-world sample of acute inpatients affected by and treated for severe mental illness. A secondary aim was to verify whether putative risk factors for QTc prolongation are confirmed in a real-world sample.
METHODS
Study Design
This study was a cross-sectional analysis of a cohort of patients with severe mental illness.
Participants
Among 898 patients admitted to the acute inpatient psychiatry unit of the psychiatry clinic at the Hospital of Padua (Padua, Italy) between July 1, 2017, and July 22, 2019, 597 patients with a valid electrocardiogram (ECG) performed during the hospitalization were included in the study. The severity of the patients’ conditions is variable; they first pass through the emergency department and are then admitted to the inpatient unit. The setting is representative of Italian psychiatric inpatient units.
Source and Variables
Data were collected through electronic medical records. Age, sex, height (cm), body weight (kg), body mass index (BMI = kg/m2), Clinical Global Impressions–Severity of Illness16 (CGI-S) scores, systolic and diastolic blood pressure (mm Hg), and blood test results were extracted. A medical history was also collected from the patients’ electronic charts, and possible concomitant medical conditions were reported. The pharmacologic treatment administered the day before ECG was noted. We also collected the dosage of antipsychotics and converted it into chlorpromazine equivalents.17 Based on available literature,2,18–20 antipsychotics were divided in relation to the risk of lengthening the QTc interval in 3 classes: low risk (aripiprazole, lurasidone, cariprazine, paliperidone, zuclopenthixol), moderate risk (quetiapine, perphenazine, fluphenazine, olanzapine, clotiapine, haloperidol), and high risk (chlorpromazine, promazine, clozapine, levomepromazine, ziprasidone). Long-acting injectable antipsychotics were considered as therapy administered the day before the ECG. For the sake of reporting, they were converted into daily dose equivalents.21 Antidepressants were grouped into classes: SSRIs, serotonin-norepinephrine reuptake inhibitors (SNRIs), TCAs, and “other,” which included mirtazapine, trazodone, bupropion, and vortioxetine. Based on current recommendations,22,23 at-risk antidepressants have been identified based on the risk of lengthening the QTc interval: citalopram, escitalopram, and tricyclic antidepressants (clomipramine, amitriptyline). Each patient had a diagnosis at discharge formulated according to the ICD-10.
ECG Procedure
The day of admission or the day after each patient underwent a 12-lead ECG, the QT interval was automatically calculated and corrected for heart rate according to Bazett’s formula. The ECG and QTc interval results were then studied and confirmed by a cardiologist. Unless alterations are found, the ECG is repeated after approximately 7–10 days of hospitalization, before discharge. If the QTc is lengthened instead, it is repeated sequentially over the subsequent days after treatment adjustments. If more EGGs were performed during the hospitalization, we considered the closest to admission.
Data Analysis
First, we calculated the primary outcome, namely the prevalence of QTc > 500 msec. Then, we assessed variable distribution with the Shapiro-Wilk test and tested the association between QTc length and binary (Mann-Whitney or t test depending on normality) and continuous (Pearson or Spearman correlation) variables. Furthermore, a multivariate linear regression model was created to test a model including putative risk factors for long QTc in a real-world setting. Statistical analyses were performed using Jamovi 2019 software (https://www.jamovi.org/). The level of statistical significance was set at P < .05.
RESULTS
A total of 597 patients were included in the study. Demographic, clinical, and pharmacologic characteristics are described in Table 1. The mean (SD) age of the sample was 45.7 (17.4) years, and 52.9% were female. The mean (SD) BMI was 26.1 (5.85) kg/m2. Overall, 22.1% of the patients were admitted for agitation, 23.3% for schizophrenia spectrum disorder relapse, 37.2% for mood disorder episodes, 14.6% for suicide attempt, and 2.8% for other reasons. Also, 16.6% had a substance-related disorder. Diagnosis at discharge was schizophrenia spectrum disorder for 35%, mood disorders for 48%, and other reasons for 17%.
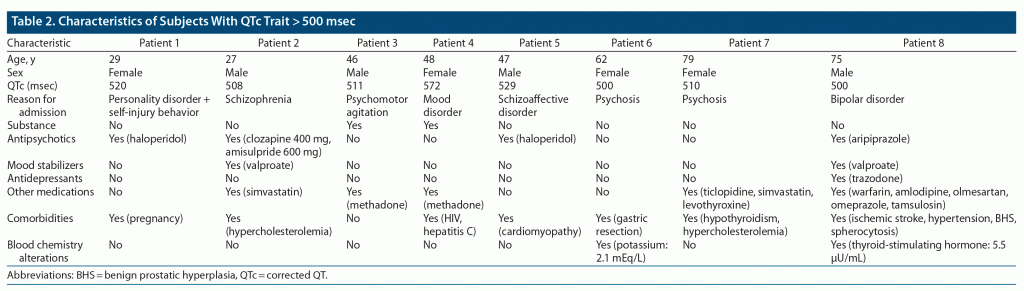
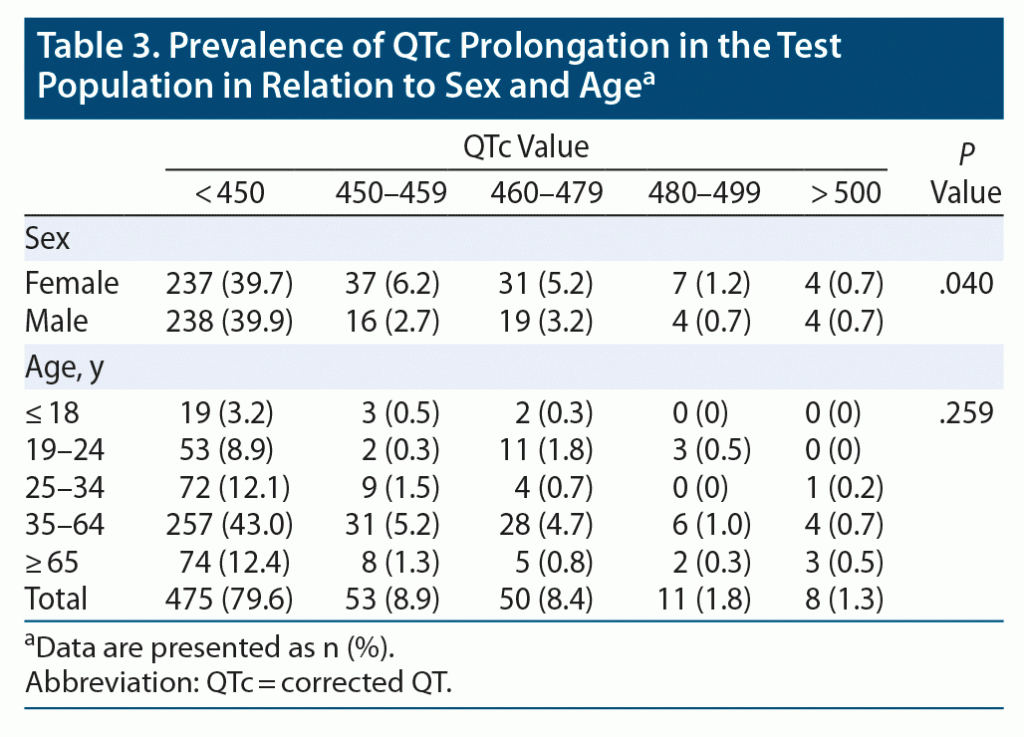
The QTc interval was > 500 msec in 1.4% of the sample; we describe the demographic, clinical, and pharmacologic characteristics of those 8 patients in Table 2. Furthermore, 11.7% of patients had a QTc > 460 msec; 3.6% of women had a QTc > 470 msec, and 7.3% of men had a QTc > 450 msec. The mean ± SD QTc was 429 ± 26.7 msec. The QTc interval was divided into 5 groups, and its distribution is reported in Table 3.
Also, prolonged QT distribution differed according to demographic factors, namely sex (χ2 = 10.0, P = .040) and age group (χ2 = 19.2, P = .259) (Table 3). Prevalence of QTc prolongation was not different based on antipsychotic QTc prolongation risk groups (χ2 = 10.3, P = .242) (Table 4).
Data on psychiatric and medical treatments were collected, including drugs at risk of QTc prolongation like methadone. There were 13 patients in methadone treatment; of these, 2 patients had a QTc > 500 msec, 3 patients had a QTc between 450 and 499 msec (459, 471, and 480 msec, respectively), and 8 patients had a QTc < 450 msec.
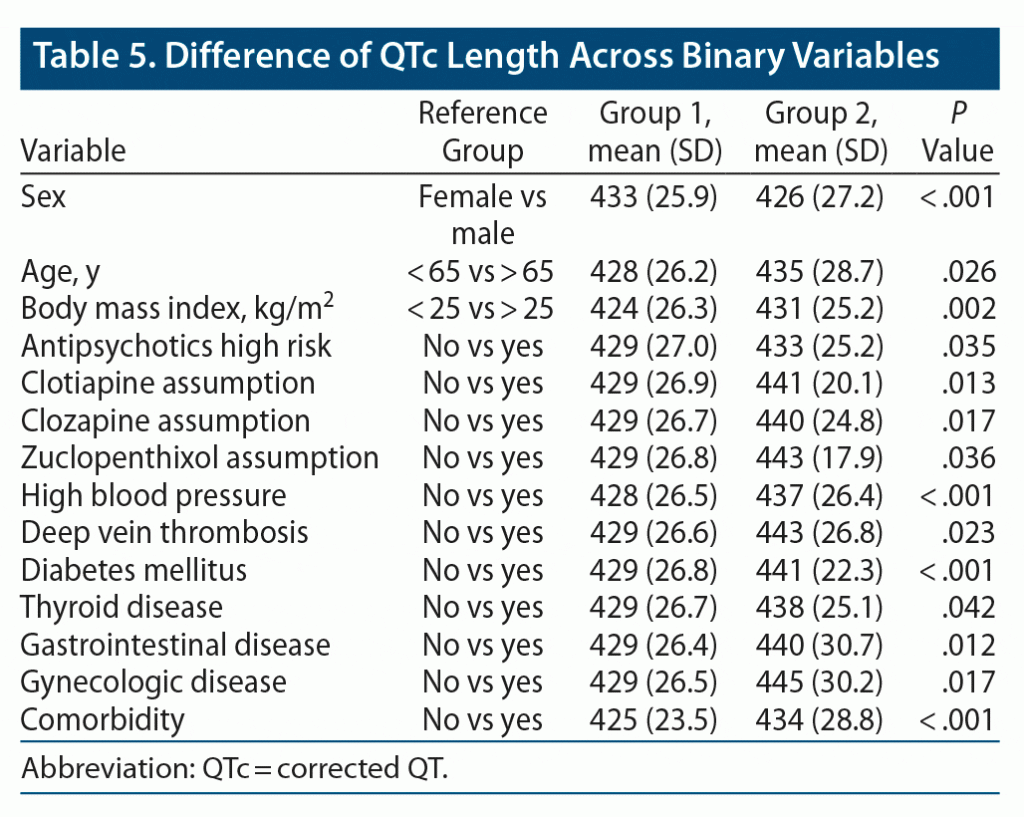
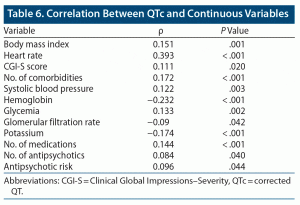
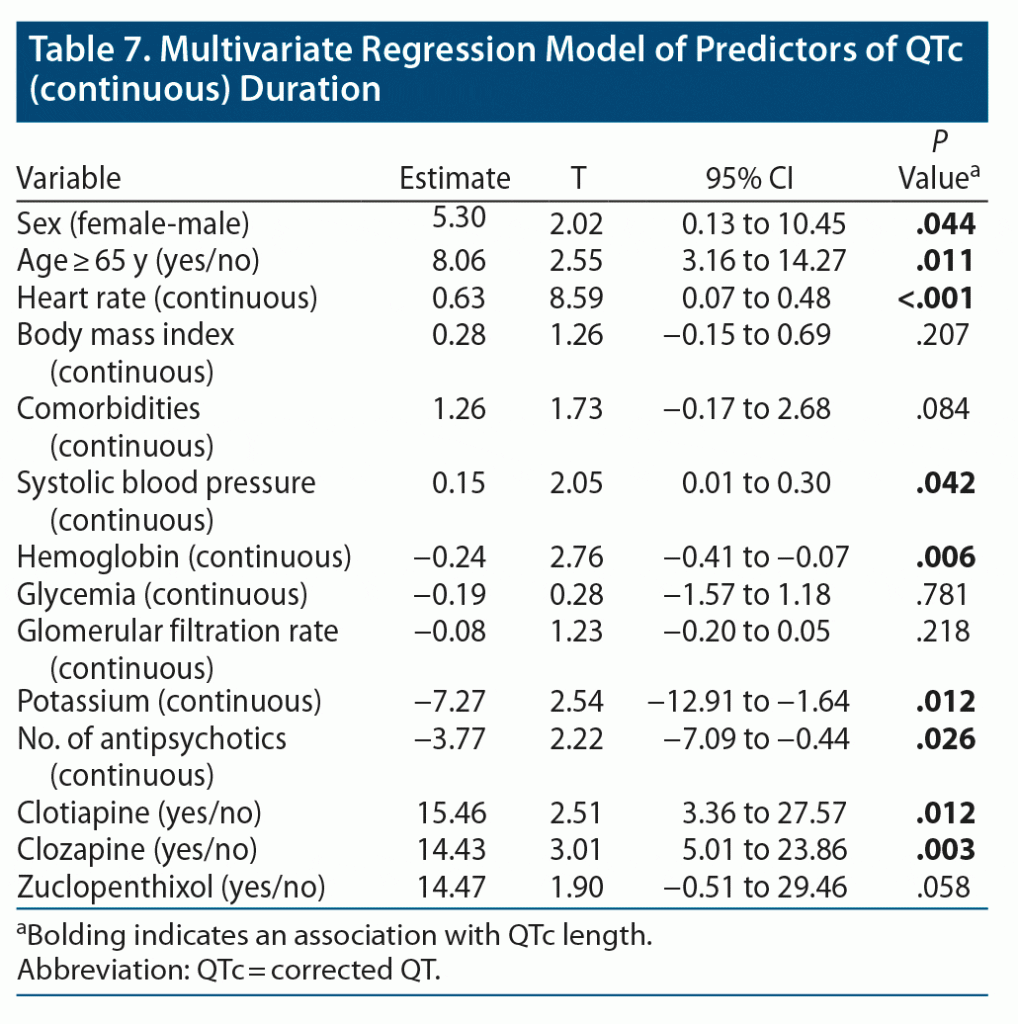
In the univariate analyses (Table 5), the QTc was longer in females (433 ± 25.9 vs 426 ± 27.2, P < .001) and in subjects aged > 65 years (428 ± 26.2 vs 435 ± 28.7, P = .026). QTc length was also significantly correlated with BMI (ρ = 0.151, P = .001), heart rate (ρ = 0.393, P < .001), clinical severity as measured with the CGI-S (ρ = 0.111, P = .020), and other variables reported in Table 6. The multivariate regression model (R2 = 31.7%) confirmed that female sex (β = 5.30 P = .044), age > 65 years (β = 8.06, P = .011), heart rate (β = 0.62, P < .001), systolic blood pressure (β = 0.15, P = .042), hemoglobin (β = −0.24, P = .006), potassium (β = −7.27, P = .012), lower antipsychotic number (β = −3.77, P = .026), clotiapine (β = 15.46, P = .012), and clozapine (β = 14.43, P = .003) were associated with QTc prolongation (Table 7).
DISCUSSION
The present study shows that female sex, age > 65 years, heart rate, systolic blood pressure, potassium, and hemoglobin were positively associated with QTc prolongation in the multivariate model. Also, only 2 antipsychotics, clozapine and clotiapine, were associated with QTc prolongation, while the others showed no statistical or clinical effect on QTc. Moreover, polypharmacotherapy with antipsychotics was not associated with increased risk of QTc prolongation.
The results of this study are relevant for the following reasons. First, they provide real-world evidence that clinically relevant QTc prolongation is a rare event that occurs in subjects with predisposing unmodifiable risk factors such as older age and female sex, which is a finding that is consistent with previous literature.4,24–27 Our study showed a low prevalence of QTc interval prolongation > 500 msec (only 1.4%). A larger percentage of patients (79.6%) had a QTc interval > 450 msec. These data agree with that of the literature,28 wherein the prevalence of QTc > 500 msec is between 0.9%29 and 2.6%.30 An increase in the QTc with age may be due to several factors. The aging process may affect the molecular determinants of the QT interval or alter the myocardium with increased myocardial fibrosis.31 Aging is also associated with alterations in the amount of sympathetic and parasympathetic tone,32 which can alter myocardial repolarization and the duration of the QTc.33,34 According to previous literature, women are at higher risk of drug-induced TdP than men.35 Sex hormones modulate QTc and contribute to the longer QTc observed in the general population of women versus men and androgenized women.36,37 Although the exact mechanisms underlying the influence of sex hormones on the repolarization and QTc interval are complex and still unresolved, androgens seem to have a protective role. Testosterone decreases the L-type calcium current and increases the potassium channel currents, resulting in a shorter QTc interval observed in both animal and human studies.38
Second, our results confirm previous findings about the role of hypokalemia on QT interval prolongation.39 Potassium channel conductance decreases with decreasing extracellular serum potassium, leading to QTc prolongation40–42 due to several factors. Hypokalemia may prolong the QT by activating calcium/calmodulin-dependent protein kinase and thereby increasing late sodium current.43 Another important underlying mechanism is that the amplitude of rapid delayed rectifier (IKr) activated by depolarization to plateau potentials decreases as extracellular potassium is lowered. This unusual behavior reflects the very fast inactivation that open Kv11.1 channels undergo such that, with depolarizing pulses, channels are distributed between open and inactivated states. Decreasing extracellular potassium shifts this balance toward occupancy of inactivated states and thus decreases overall repolarizing current.44 Further, the drug block of open channels is enhanced with low extracellular potassium, thereby further enhancing QT prolongation.43
Third, polypharmacotherapy does not seem to increase the risk of QTc prolongation, which is a result in contrast with previous literature.2,4,10,26 In the literature, there are conflicting findings on antipsychotic polypharmacy and its role with respect to the QTc interval. Some research suggests that polypharmacy may be associated with an increased risk since greater cumulative doses would be given, thus suggesting a mainly dose-related action.45 Other studies26 conversely report a lower QT interval for patients receiving antipsychotic polypharmacy. Fourth, the dose-dependency ratio was not confirmed in our study,46 probably because very high doses were hardly reached.
Regarding the specific role of medications, we found no increased risk with haloperidol,47 which could be explained by the low doses and oral administration to comply with current safety warnings.12 Aripiprazole was found to be safe, confirming data from previous literature,47,48 as was lurasidone.18 We also found no increased risk for long-acting formulations, which is in contrast with the study by Chong et al,49 in which FGA long-acting drugs (fluphenazine and flupentixol) were used. In our study, clotiapine, an antipsychotic with the structure and properties of dibenzothiazepines similar to those of phenothiazines, appears to be significantly correlated with QTc lengthening.29,50 Clozapine, which in our analysis correlated significantly with QTc prolongation, has been associated with an increased risk of sudden cardiac death,3 but only rarely with QTc prolongation,51–53 suggesting that another mechanism could mediate its relationship with sudden cardiac death. Since clozapine can cause myocarditis, it could act by sensitizing the myocardium to the effect of QT prolongation due to the concomitant use of other drugs.54–58 On the other hand, the lack of association between sudden cardiac death with clozapine and QTc prolongation might be due to biases and nonsystematic reporting of QTc measures. Regarding antidepressants, SSRIs, SNRIs, mirtazapine, trazodone, bupropion, and vortioxetine have proved to be safe. Citalopram and escitalopram, despite the warning data of the US Food and Drug Administration,59 were also found to be safe. TCAs, compared with other antidepressants, showed conversely a significant association with the lengthening of QTc and therefore seem to be the only antidepressants at risk for these conditions.60,61 Mood stabilizers, lithium, valproate, and lamotrigine were safe with respect to QTc prolongation.3
Fifth, an important role seems to be played by medical comorbidities. According to our study, hypertension (also emerged from the correlation with systolic blood pressure)50,62 and diabetes mellitus (and glycemia)63–65 are associated with QTc prolongation. Our data also revealed an association with kidney function (expressed in terms of glomerular filtration rate)66 and values of hemoglobin.
Despite the absence of TdP in our sample and the low incidence of TdP and QT in the general and psychiatric population, it should be emphasized that a risk exists, but that it is low in absolute terms and can be effectively reduced by adequate risk stratification.66 Before starting antipsychotic treatment, an ECG should be recorded and examined. This is particularly important in subjects with established cardiovascular diseases or when a high-risk medication or parenteral therapy is considered.67 Because over 85% of patients with drug-induced QT interval prolongation have 2 or more additional risk factors,29 it is important to undertake a careful analysis of the concomitant risk factors to reduce risk: undertake a thorough medical and pharmacologic history, review the list of drugs that the patient takes, identify concomitant medical comorbidities, and monitor blood electrolyte levels.54,68,69
The present study has several limitations. First, the real-world nature of data, which can be considered a strength of the work, also has inherent limitations such as lack of systematic collection of potential confounding factors, including smoking, calcium, and magnesium levels. Second, regarding antipsychotics, only a few patients were taking thioridazine, pimozide, sulpiride, droperidol, and ziprasidone, which have a higher QTc prolongation risk. Third, the cross-sectional design of the study limits any causal inference.
In conclusion, QTc prolongation seems to be a rare occurrence that affects only a small portion of the psychiatric population and is explained by demographic, clinical, and pharmacologic factors in one-third of these patients. Factors mostly implicated in the risk are unchangeable, such as age and sex, or are secondary to general medical conditions. Treatment with psychiatric drugs, on the other hand, would seem to have a marginal role.
Submitted: January 5, 2021; accepted May 6, 2021.
Published online: February 17, 2022.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- QTc interval prolongation is a rare event associated with identifiable factors.
- Consideration of the risk factors associated with QTc prolongation helps to minimize the risk of a critical event.
References (69)

- Huhn M, Nikolakopoulou A, Schneider-Thoma J, et al. Comparative efficacy and tolerability of 32 oral antipsychotics for the acute treatment of adults with multi-episode schizophrenia: a systematic review and network meta-analysis. Lancet. 2019;394(10202):939–951. PubMed CrossRef
- Beach SR, Celano CM, Sugrue AM, et al. QT prolongation, torsades de pointes, and psychotropic medications: a 5-year update. Psychosomatics. 2018;59(2):105–122. PubMed CrossRef
- Beach SR, Celano CM, Noseworthy PA, et al. QTc prolongation, torsades de pointes, and psychotropic medications. Psychosomatics. 2013;54(1):1–13. PubMed CrossRef
- Taylor DM. Antipsychotics and QT prolongation. Acta Psychiatr Scand. 2003;107(2):85–95. PubMed CrossRef
- Gupta A, Lawrence AT, Krishnan K, et al. Current concepts in the mechanisms and management of drug-induced QT prolongation and torsade de pointes. Am Heart J. 2007;153(6):891–899. PubMed CrossRef
- Dargani NV, Malhotra AK. Safety profile of iloperidone in the treatment of schizophrenia. Expert Opin Drug Saf. 2014;13(2):241–246. PubMed CrossRef
- Ames D, Camm J, Cook P, et al; Cardiac Safety in Schizophrenia Group. Minimizing the risks associated with QTc prolongation in people with schizophrenia: a consensus statement by the Cardiac Safety in Schizophrenia Group. Encephale. 2002;28(6 Pt 1):552–562. PubMed CrossRef
- Nielsen J, Wang F, Graff C, et al. QT dynamics during treatment with sertindole. Ther Adv Psychopharmacol. 2015;5(1):26–31. PubMed CrossRef
- Murray-Thomas T, Jones ME, Patel D, et al. Risk of mortality (including sudden cardiac death) and major cardiovascular events in atypical and typical antipsychotic users: a study with the general practice research database. Cardiovasc Psychiatry Neurol. 2013;2013:247486. PubMed CrossRef
- Mackin P. Cardiac side effects of psychiatric drugs. Hum Psychopharmacol. 2008;23(suppl 1):3–14. PubMed CrossRef
- Minns AB, Clark RF. Toxicology and overdose of atypical antipsychotics. J Emerg Med. 2012;43(5):906–913. PubMed CrossRef
- Meyer-Massetti C, Cheng CM, Sharpe BA, et al. The FDA extended warning for intravenous haloperidol and torsades de pointes: how should institutions respond? J Hosp Med. 2010;5(4):E8–E16. PubMed CrossRef
- Fayssoil A, Issi J, Guerbaa M, et al. Torsade de pointes induced by citalopram and amiodarone. Ann Cardiol Angeiol (Paris). 2011;60(3):165–168. PubMed CrossRef
- Marano G, Traversi G, Romagnoli E, et al. Cardiologic side effects of psychotropic drugs. J Geriatr Cardiol. 2011;8(4):243–253. PubMed
- Mitchell JE, Mackenzie TB. Cardiac effects of lithium therapy in man: a review. J Clin Psychiatry. 1982;43(2):47–51. PubMed CrossRef
- Guy W. Clinical Global Impressions. ECDEU Assessment Manual for Psychopharmacology. DHEW Publication No. 76-338. Rockville, MD: National Institute of Mental Health; 1976:217–222.
- Woods SW. Chlorpromazine equivalent doses for the newer atypical antipsychotics. J Clin Psychiatry. 2003;64(6):663–667. PubMed CrossRef
- Leucht S, Cipriani A, Spineli L, et al. Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis. Lancet. 2013;382(9896):951–962. PubMed CrossRef
- Supplement to: Leucht S, Cipriani A, Spineli L, et al. Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis Lancet 2013; published online June 27. http://dx.doi.org/10.1016/S0140-6736(13)60733-3Leucht S. Supplementary Appendix. Lancet Diabetes Endocrinol. 2015;3:925–927.
- Carrà G, Crocamo C, Bartoli F, et al; STAR Network Group. First-generation antipsychotics and QTc: any role for mediating variables? Hum Psychopharmacol. 2016;31(4):313–318. PubMed CrossRef
- Rothe PH, Heres S, Leucht S. Dose equivalents for second generation long-acting injectable antipsychotics: the minimum effective dose method. Schizophr Res. 2018;193:23–28. PubMed CrossRef
- US Food and Drug Administration. E14 Clinical Evaluation of QT/QTc Interval Prolongation and Proarrhythmic Potential for Non-Antiarrhythmic Drugs Questions and Answers (R3) Guidance for Industry. June 2017. www.fda.gov/regulatory-information/search-fda-guidance-documents/e14-clinical-evaluation-qtqtc-interval-prolongation-and-proarrhythmic-potential-non-antiarrhythmic-1
- FDA. Guidance for Industry Interval Prolongation and Guidance for Industry. E14 Clinical Evaluation of QT/QTc Interval Prolongation and Proarrythmic Potential for Non-Antiarrhythmic Drugs. US Dep Health Hum Serv Food Drug Adm Cent Drug Eval Res CDER Cent Biol Eval Res CBER; 2005:1–16.
- Rautaharju PM, Manolio TA, Psaty BM, et al; Cardiovascular Health Study Collaborative Research Group. Correlates of QT prolongation in older adults (the Cardiovascular Health Study). Am J Cardiol. 1994;73(13):999–1002. PubMed CrossRef
- Vieweg WVR, Wood MA, Fernandez A, et al. Proarrhythmic risk with antipsychotic and antidepressant drugs: implications in the elderly. Drugs Aging. 2009;26(12):997–1012. PubMed CrossRef
- Mackin P, Young AH. QTc interval measurement and metabolic parameters in psychiatric patients taking typical or atypical antipsychotic drugs: a preliminary study. J Clin Psychiatry. 2005;66(11):1386–1391. PubMed CrossRef
- Lubart E, Segal R, Yearovoi A, et al. QT interval disturbances in hospitalized elderly patients. Isr Med Assoc J. 2009;11(3):147–150. PubMed
- Nosè M, Bighelli I, Castellazzi M, et al; STAR NETWORK GROUP. Prevalence and correlates of QTc prolongation in Italian psychiatric care: cross-sectional multicentre study. Epidemiol Psychiatr Sci. 2016;25(6):532–540. PubMed CrossRef
- Girardin FR, Gex-Fabry M, Berney P, et al. Drug-induced long QT in adult psychiatric inpatients: the 5-year cross-sectional ECG Screening Outcome in Psychiatry study. Am J Psychiatry. 2013;170(12):1468–1476. PubMed CrossRef
- Pasquier M, Pantet O, Hugli O, et al. Prevalence and determinants of QT interval prolongation in medical inpatients. Intern Med J. 2012;42(8):933–940. PubMed CrossRef
- Liu CY, Liu YC, Wu C, et al. Evaluation of age-related interstitial myocardial fibrosis with cardiac magnetic resonance contrast-enhanced T1 mapping: MESA (Multi-Ethnic Study of Atherosclerosis). J Am Coll Cardiol. 2013;62(14):1280–1287. PubMed CrossRef
- Pfeifer MA, Weinberg CR, Cook D, et al. Differential changes of autonomic nervous system function with age in man. Am J Med. 1983;75(2):249–258. PubMed CrossRef
- Can I, Aytemir K, Köse S, et al. Physiological mechanisms influencing cardiac repolarization and QT interval. Card Electrophysiol Rev. 2002;6(3):278–281. PubMed CrossRef
- Rabkin SW, Cheng XJ, Thompson DJS. Detailed analysis of the impact of age on the QT interval. J Geriatr Cardiol. 2016;13(9):740–748. PubMed
- Salem JE, Dureau P, Bachelot A, et al. Association of oral contraceptives with drug-induced QT interval prolongation in healthy nonmenopausal women. JAMA Cardiol. 2018;3(9):877–882. PubMed CrossRef
- Salem JE, Alexandre J, Bachelot A, et al. Influence of steroid hormones on ventricular repolarization. Pharmacol Ther. 2016;167:38–47. PubMed CrossRef
- Abehsira G, Bachelot A, Badilini F, et al. Complex influence of gonadotropins and sex steroid hormones on QT interval duration. J Clin Endocrinol Metab. 2016;101(7):2776–2784. PubMed CrossRef
- Vink AS, Clur SB, Wilde AAM, et al. Effect of age and gender on the QTc-interval in healthy individuals and patients with long-QT syndrome. Trends Cardiovasc Med. 2018;28(1):64–75. PubMed CrossRef
- Trojak B, Astruc K, Pinoit JM, et al. Hypokalemia is associated with lengthening of QT interval in psychiatric patients on admission. Psychiatry Res. 2009;169(3):257–260. PubMed CrossRef
- Noble D, Tsien RW. The kinetics and rectifier properties of the slow potassium current in cardiac Purkinje fibres. J Physiol. 1968;195(1):185–214. PubMed CrossRef
- Yang T, Roden DM. Extracellular potassium modulation of drug block of IKr: implications for torsade de pointes and reverse use-dependence. Circulation. 1996;93(3):407–411. PubMed CrossRef
- Marill KA, Miller ES. Hypokalemia in women and methadone therapy are the strongest non-cardiologic factors associated with QT prolongation in an emergency department setting. J Electrocardiol. 2017;50(4):416–423. PubMed CrossRef
- Roden DM. Predicting drug-induced QT prolongation and torsades de pointes. J Physiol. 2016;594(9):2459–2468. PubMed CrossRef
- Yang T, Snyders DJ, Roden DM. Rapid inactivation determines the rectification and [K+]o dependence of the rapid component of the delayed rectifier K+ current in cardiac cells. Circ Res. 1997;80(6):782–789. PubMed CrossRef
- John AP, Dragovic M. Antipsychotic polypharmacy is not associated with reduced dose of individual antipsychotics in schizophrenia. J Clin Psychopharmacol. 2015;35(2):193–195. PubMed CrossRef
- Correll CU, Harris J, Figen V, et al. Antipsychotic drug administration does not correlate with prolonged rate-corrected QT interval in children and adolescents: results from a nested case-control study. J Child Adolesc Psychopharmacol. 2011;21(4):365–368. PubMed CrossRef
- Barbui C, Bighelli I, Carrà G, et al; STAR NETWORK INVESTIGATORS. Antipsychotic dose mediates the association between polypharmacy and corrected QT interval. PLoS One. 2016;11(2):e0148212. PubMed CrossRef
- Polcwiartek C, Sneider B, Graff C, et al. The cardiac safety of aripiprazole treatment in patients at high risk for torsade: a systematic review with a meta-analytic approach. Psychopharmacology (Berl). 2015;232(18):3297–3308. PubMed CrossRef
- Chong SA, Mythily A, Lum A, et al. Prolonged QTc intervals in medicated patients with schizophrenia. Hum Psychopharmacol. 2003;18(8):647–649. PubMed CrossRef
- Ramos-Ríos R, Arrojo-Romero M, Paz-Silva E, et al. QTc interval in a sample of long-term schizophrenia inpatients. Schizophr Res. 2010;116(1):35–43. PubMed CrossRef
- Kang UG, Kwon JS, Ahn YM, et al. Electrocardiographic abnormalities in patients treated with clozapine. J Clin Psychiatry. 2000;61(6):441–446. PubMed CrossRef
- Xiang YT, Chiu HFK, Ungvari GS, et al. QTc prolongation in schizophrenia patients in Asia: clinical correlates and trends between 2004 and 2008/2009. Hum Psychopharmacol. 2015;30(2):94–99. PubMed CrossRef
- Washington NB, Brahm NC, Kissack J. Which psychotropics carry the greatest risk of QTc prolongation? Curr Psychiatr. 2012;11:36–39.
- Wenzel-Seifert K, Wittmann M, Haen E. QTc prolongation by psychotropic drugs and the risk of torsade de pointes. Dtsch Arztebl Int. 2011;108(41):687–693. PubMed CrossRef
- Poluzzi E, Raschi E, Moretti U, et al. Drug-induced torsades de pointes: data mining of the public version of the FDA Adverse Event Reporting System (AERS). Pharmacoepidemiol Drug Saf. 2009;18(6):512–518. PubMed CrossRef
- Ray WA, Chung CP, Murray KT, et al. Atypical antipsychotic drugs and the risk of sudden cardiac death. N Engl J Med. 2009;360(3):225–235. PubMed CrossRef
- Warner B, Hoffmann P. Investigation of the potential of clozapine to cause torsade de pointes. Adverse Drug React Toxicol Rev. 2002;21(4):189–203. PubMed CrossRef
- Agelink MW, Majewski T, Wurthmann C, et al. Effects of newer atypical antipsychotics on autonomic neurocardiac function: a comparison between amisulpride, olanzapine, sertindole, and clozapine. J Clin Psychopharmacol. 2001;21(1):8–13. PubMed CrossRef
- FDA Drug Safety Communication: Revised Recommendations for Celexa (citalopram hydrobromide) Related to a Potential Risk of Abnormal Heart rhythms With High Doses. Accessed January 12, 2022. https://www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-revised-recommendations-celexa-citalopram-hydrobromide-related
- Reilly JG, Ayis SA, Ferrier IN, et al. QTc-interval abnormalities and psychotropic drug therapy in psychiatric patients. Lancet. 2000;355(9209):1048–1052. PubMed CrossRef
- van Noord C, Straus SMJM, Sturkenboom MCJM, et al. Psychotropic drugs associated with corrected QT interval prolongation. J Clin Psychopharmacol. 2009;29(1):9–15. PubMed CrossRef
- Schillaci G, Pirro M, Ronti T, et al. Prognostic impact of prolonged ventricular repolarization in hypertension. Arch Intern Med. 2006;166(8):909–913. PubMed CrossRef
- Naas AAO, Davidson NC, Thompson C, et al. QT and QTc dispersion are accurate predictors of cardiac death in newly diagnosed non-insulin dependent diabetes: cohort study. BMJ. 1998;316(7133):745–746. PubMed CrossRef
- Veglio M, Sivieri R, Chinaglia A, et al. QT interval prolongation and mortality in type 1 diabetic patients: a 5-year cohort prospective study. Neuropathy Study Group of the Italian Society of the Study of Diabetes, Piemonte Affiliate. Diabetes Care. 2000;23(9):1381–1383. PubMed CrossRef
- Festa A, D’Agostino R Jr, Rautaharju P, et al. Relation of systemic blood pressure, left ventricular mass, insulin sensitivity, and coronary artery disease to QT interval duration in nondiabetic and type 2 diabetic subjects. Am J Cardiol. 2000;86(10):1117–1122. PubMed CrossRef
- Gross JL, Friedman R, Azevedo MJ, et al. Effect of age and sex on glomerular filtration rate measured by 51Cr-EDTA. Braz J Med Biol Res. 1992;25(2):129–134. PubMed
- Shah AA, Aftab A, Coverdale J. QTc prolongation with antipsychotics: is routine ECG monitoring recommended? J Psychiatr Pract. 2014;20(3):196–206. PubMed CrossRef
- Haverkamp W, Deuschle M. Lengthening of QT interval by antipsychotic drugs. Nervenarzt. 2006;77(3):276, 278–280, 282–284 passim. PubMed CrossRef
- Stöllberger C, Huber JO, Finsterer J. Antipsychotic drugs and QT prolongation. Int Clin Psychopharmacol. 2005;20(5):243–251. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!