Functional vomiting is frequently associated with psychiatric comorbidity, though the evidence for association is inconsistent. There is no clear guideline for management, and a trial of antidepressants and psychological measures are often used.1,2 Here, we discuss the cases of 2 patients who responded to a biofeedback-based behavioral intervention.
Case 1
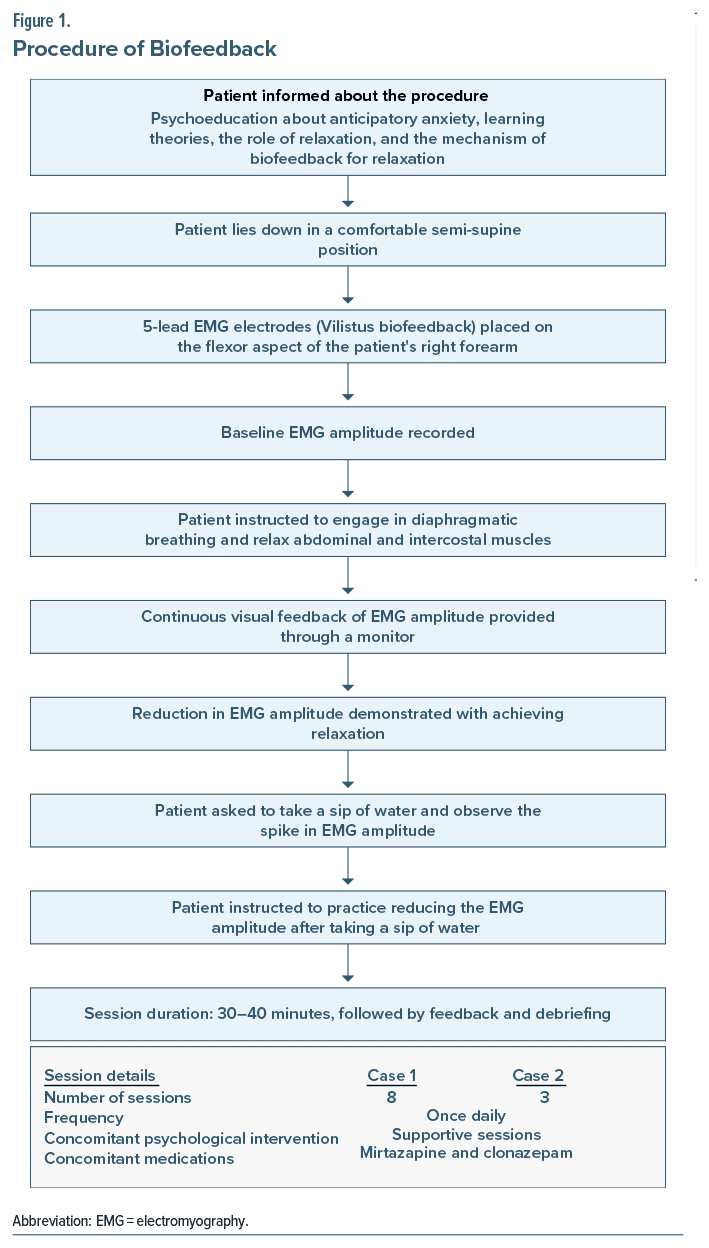
A 22-year-old married woman presented with a 5-year illness duration starting after postappendectomy surgical site infection, with subsequent nausea and vomiting (3–4 times/day) after meals. The nonprojectile vomit consisted of recently ingested food devoid of bile or blood and accompanied by dull-aching epigastric pain lasting nearly an hour. There was no fever, diarrhea, or constipation. Over time, she also started experiencing occasional loss of consciousness during vomiting (once or twice a month) without abnormal limb movements, frothing, or incontinence. Despite several consultations, her symptoms persisted. She withdrew from college due to anticipatory anxiety regarding vomiting and reduced food intake, leading to weight loss. Following an upper gastrointestinal endoscopy, no active intervention was advised, and she was referred for psychiatric consultation by a gastroenterologist. Initially, she was prescribed mirtazapine 15 mg, pantoprazole 40 mg, and domperidone 20 mg for 4 weeks. She had negative affectivity traits (as per ICD-11) and a family history of bodily distress disorder (vomiting as one of the symptoms) in her father. The psychological exploration (including projective testing) yielded no stressors. She was hospitalized for further management, as supportive sessions and relaxation exercises failed, and a trial of electromyography biofeedback was given (Figure 1). During the initial 3 sessions, the patient vomited shortly after the session; vomiting was delayed for 30–60 minutes after the subsequent 2 sessions and ceased entirely thereafter. The type of meal was changed in the sessions from liquid to light snacks.
Case 2
A 20-year-old woman presented to the gastroenterologist with an 8-year history of recurrent vomiting, with the current episode lasting for the past 3 months. Organic causes were ruled out, and she was referred for psychiatric consultation. Preparing for competitive exams coincided with the onset of the current episode. Vomiting occurred within a few minutes after eating or drinking anything 10–15 times a day and contained recently ingested food. She also experienced sleep disturbances and significant weight loss. No mood or anxiety symptoms or eating disorders were present. The family history was negative. She had similar episodes every year for 2–3 months, with no identifiable stressors. She received a trial of escitalopram, duloxetine, and levosulpiride. Personality assessment revealed high negative affectivity traits. She was prescribed mirtazapine up to 22.5 mg and clonazepam 0.5 mg with relaxation training and was hospitalized subsequently due to nonresponse. Psychometric assessments and sessions revealed no stressors. Subsequently, electromyography-guided biofeedback was tried. Her vomiting episodes ceased after 3 sessions.
Discussion
In both cases, the patient was a young woman with no identifiable organic cause or stressor, negative affectivity traits, and lack of prominent psychological symptoms (unable to establish a psychiatric diagnosis). The first case had a continuous course, while the second was episodic. It is reported that patterns may vary with psychological conditions, ie, dissociation often presents with continuous vomiting, while depression and anxiety involve irregular or postprandial patterns.3
The lack of any prominent stressor and response to behavioral intervention supports the possibility that vomiting, initially caused by a physical issue, can become a learned behavior, supporting behavioral etiological theories.4 Biofeedback is also effective in rumination disorder5 and cyclic vomiting syndrome,6 indicating a pathophysiologic similarity, ie, patients may develop a reflex response of abdominal muscle contraction and lower esophageal sphincter relaxation after a meal. Biofeedback can provide clinicians with a vital treatment alternative and an avenue to elucidate the pathophysiology of functional vomiting.
Article Information
Published Online: March 11, 2025. https://doi.org/10.4088/PCC.24cr03829
© 2025 Physicians Postgraduate Press, Inc.
Prim Care Companion CNS Disord 2025;27(2):24cr03829
Submitted: August 12, 2024; accepted December 17, 2024.
To Cite: Kaur H, Gupta C, Biswas S, et al. Biofeedback for the management of patients with functional vomiting. Prim Care Companion CNS Disord 2025;27(2):24cr03829
Author Affiliations: Department of Psychiatry, Institute of Human Behaviour and Allied Sciences, Delhi, India (Kaur); Department of Psychiatry, All India Institute of Medical Sciences, Jodhpur, Rajasthan, India (Gupta, Biswas, Swami).
Corresponding Author: Mukesh Kumar Swami, MD, Department of Psychiatry, All India Institute of Medical Sciences, Basni Industrial Area, MIA 2nd Phase, Basni, Jodhpur, Rajasthan 342005 ([email protected]).
Relevant Financial Relationships: None.
Funding/Support: None.
Patient Consent: Consent was received from the patients to publish the case reports, and the information has been de-identified to protect patient anonymity.
ORCID: Mukesh Kumar Swami: https://orcid.org/0000-0001-9870-8397
References (6)

- Olden KW, Chepyala P. Functional nausea and vomiting. Nat Clin Pract Gastroenterol Hepatol. 2008;5(4):202–208. PubMed CrossRef
- Rosenthal RH, Webb WL, Wruble LD. Diagnosis and management of persistent psychogenic vomiting. Psychosomatics. 1980;21(9):722–730. PubMed CrossRef
- Muraoka M, Mine K, Matsumoto K, et al. Psychogenic vomiting: the relation between patterns of vomiting and psychiatric diagnoses. Gut. 1990;31(5):526–528. PubMed CrossRef
- Pazulinec R, Sajwaj T. Psychological treatment approaches to psychogenic vomiting and rumination. In: Hölzl R, Whitehead WE, eds. Psychophysiology of the Gastrointestinal Tract. Springer; 1983.
- Barba E, Burri E, Accarino A, et al. Biofeedback-guided control of abdominothoracic muscular activity reduces regurgitation episodes in patients with rumination. Clin Gastroenterol Hepatol. 2015;13(1):100–106.e1.n CrossRef
- Slutsker B, Konichezky A, Gothelf D. Breaking the cycle: cognitive behavioral therapy and biofeedback training in a case of cyclic vomiting syndrome. Psychol Health Med. 2010;15(6):625–631. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!